Chronic Sinusitis for Years: Causes, Symptoms, and Treatment Options
If Your Sinus Symptoms Won’t Go Away, You’re Not Alone
Living with constant nasal congestion, facial pressure, postnasal drip, reduced sense of smell, and fatigue can wear you down—especially when it feels like nothing ever fully clears. If you’ve had chronic sinusitis for years, it helps to know two things: this problem is common, and it’s often manageable once the underlying drivers are identified.
Think of it less like a cold that never ends and more like a long-running cycle of inflammation and poor drainage. This article explains why symptoms can linger for months (or even years), what an evidence-based evaluation usually includes, and the treatment options ENT specialists often use to improve long-term control. If you’re still sorting out whether your symptoms match sinus disease, you can also review common symptoms of sinus problems: https://sleepandsinuscenters.com/symptoms-of-sinus-problems.
— A persistent pattern of nasal inflammation and impaired drainage is usually the core problem, and it can be treated once identified. —
What Is “Chronic Sinusitis” (Chronic Rhinosinusitis)?
Chronic sinusitis is more accurately called chronic rhinosinusitis (CRS), a condition defined by long-lasting symptoms and ongoing inflammation rather than a single prolonged infection.

The 12-week rule (what “chronic” means)
Chronic sinusitis is more accurately called chronic rhinosinusitis (CRS). Most guidelines define CRS by symptoms that last longer than 12 weeks—not a stubborn cold or a single bad allergy season (EPOS 2020).
Chronic vs. recurrent sinus infections (quick clarification)
- Chronic rhinosinusitis (CRS): ongoing inflammation and symptoms that wax and wane but don’t fully resolve
- Recurrent acute sinusitis: separate infection episodes with more normal breathing and minimal symptoms in between
This distinction matters because CRS is often not just an infection that needs repeated antibiotics (AAO-HNSF).

Two main CRS “types” (why it matters for treatment)
- CRS with nasal polyps (CRSwNP)
- CRS without nasal polyps (CRSsNP)
These categories can influence choices around steroids, surgery, and biologic medications.
— In CRS, the word “chronic” refers to duration (>12 weeks) and ongoing inflammation, not just repeated infections. —
Symptoms of Chronic Sinusitis (What It Can Feel Like)
Core symptoms clinicians look for
- Nasal blockage/congestion
- Nasal drainage (runny nose and/or postnasal drip)
- Facial pressure/pain (not always present)
- Reduced smell and/or taste
These symptoms, together with objective findings on exam, nasal endoscopy, or imaging, support a CRS diagnosis (EPOS 2020). Many people describe a pattern of feeling partially better for a few days, then slipping back into congestion and drainage.
Other common “years-long” symptoms people report
- Chronic cough, throat clearing, or hoarseness from drainage
- Bad breath
- Ear pressure or fullness
- Poor sleep, fatigue, and trouble concentrating
- Symptoms that worsen with allergies, smoke, strong odors, weather shifts, or respiratory infections
When symptoms are less likely to be sinus-related
Not all “sinus pressure” is truly sinus disease. Conditions that can mimic CRS include migraine or other headache disorders, TMJ dysfunction (jaw-related pain/pressure), and chronic rhinitis without sinus inflammation (nasal swelling but normal sinus imaging). That’s why a structured evaluation is so helpful—especially if you’ve had chronic sinusitis for years but haven’t had objective testing.
— If core symptoms persist and testing confirms inflammation, CRS becomes the more likely diagnosis. —
Why Chronic Sinusitis Can Last for Years (Causes + Risk Factors)
CRS is often more about chronic inflammation and impaired drainage than one infection that never goes away.
Ongoing inflammation (the most common driver)
When the lining of the nose and sinuses stays swollen, natural drainage pathways can narrow. Mucus may stagnate, symptoms persist, and flare-ups become easier to trigger. EPOS 2020 describes CRS primarily as an inflammatory condition.
Nasal polyps
Nasal polyps are benign inflammatory growths that can block airflow and drainage and are strongly associated with reduced sense of smell. Polyps can make symptoms more difficult to control without consistent anti-inflammatory treatment.
Allergies and chronic rhinitis
Seasonal or year-round allergies can add ongoing inflammation in the nasal passages. For some people, identifying allergic triggers becomes key to long-term control—especially when symptoms spike around pets, dust, or pollen seasons. If allergy symptoms are a major pattern, allergy testing may be part of the broader evaluation: https://sleepandsinuscenters.com/allergy-testing.
Structural/anatomy contributors
Anatomy can contribute to poor sinus ventilation and drainage, such as a deviated septum, enlarged turbinates, naturally narrow sinus drainage pathways, or changes after trauma or prior surgery.
Repeated infections or “flares” (not always the root cause)
Some people experience acute exacerbations on top of baseline inflammation. These flare-ups can feel like “another sinus infection,” even when the underlying issue is chronic swelling and impaired clearance.
Environmental and lifestyle triggers
Irritants can worsen nasal and sinus inflammation, including smoking/vaping exposure, air pollution or workplace irritants, strong fragrances/cleaning chemicals, and damp or mold-prone environments.
Medical conditions that can complicate CRS
CRS can overlap with other health conditions, including asthma, AERD (aspirin-exacerbated respiratory disease), immune deficiencies (more likely when infections are frequent/severe), and reflux/LPR, which may contribute to symptoms in some people, though its role in CRS is not always clear.
— Long-lasting CRS usually reflects a mix of inflammation, anatomy, and triggers—understanding your mix guides the best treatment plan. —

How Chronic Sinusitis Is Diagnosed (What to Expect at an ENT Visit)
History and symptom timeline
Because “chronic” has a specific meaning, clinicians typically ask about duration (>12 weeks), symptom pattern, triggers, prior treatments, and response to medications (including nasal sprays). Bringing a short list—what you tried, how long, and what happened—can make the visit more productive.
Nasal exam and nasal endoscopy
A detailed nasal exam—and often nasal endoscopy—can help visualize swelling, drainage, crusting, or polyps. EPOS 2020 emphasizes the need for objective evidence (not symptoms alone) to confirm CRS.
When a CT scan is useful (and when it isn’t)
A sinus CT scan can show which sinuses are inflamed and whether drainage pathways are blocked. CT is especially helpful when symptoms persist despite appropriate therapy and when procedural planning is being considered. Learn more here: https://sleepandsinuscenters.com/blog/sinus-ct-scan-what-it-shows-and-how-it-helps-diagnose-sinus-issues.
Allergy testing or additional workup (when indicated)
Depending on your history, evaluation may include allergy assessment, review of asthma control, or other targeted testing when symptoms suggest contributing conditions.
Why antibiotics aren’t automatically the answer
CRS is often inflammatory, not purely bacterial. Antibiotics are typically reserved for cases where an acute bacterial infection or bacterial exacerbation is suspected, rather than used routinely for chronic symptoms (AAO-HNSF).
— Objective findings on exam, endoscopy, or imaging confirm CRS and help tailor the right next steps. —
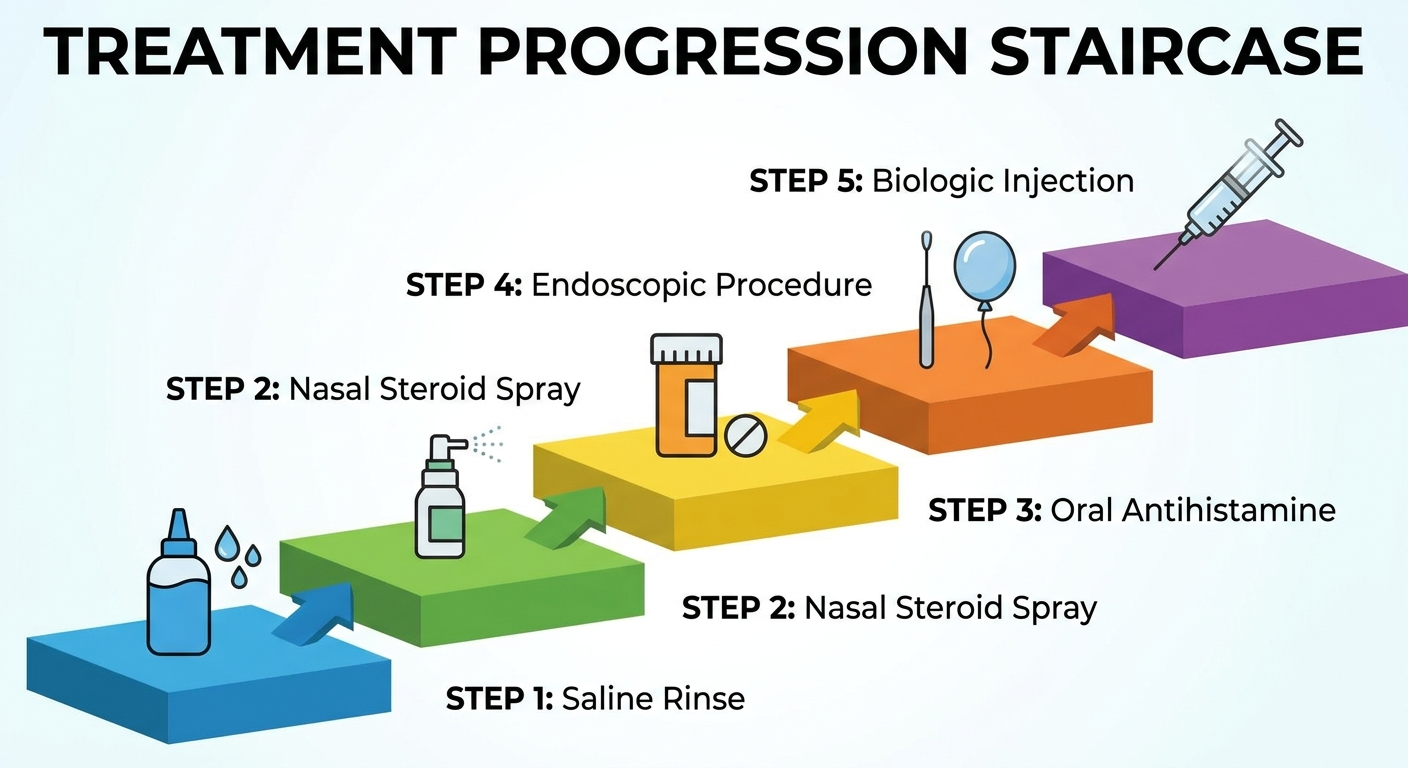
Treatment Options (Stepwise, Evidence-Based)
Many people with chronic sinusitis for years do best with a stepwise plan—starting with foundational daily therapies and escalating based on objective findings and response.
Foundation therapies (often first-line and long-term)
- Saline nasal irrigation: Helps rinse mucus and irritants and supports nasal hygiene. Use distilled/sterile water or properly boiled and cooled water.
- Intranasal corticosteroids: Reduce inflammation over time; consistency matters for effectiveness. These are core therapies in EPOS 2020.
Addressing allergies and triggers
- Antihistamines and an individualized allergy plan are most helpful when allergies are a clear trigger.
- Environmental control can reduce irritant exposure (see Lifestyle Tips below).
- More on overall care pathways: https://sleepandsinuscenters.com/chronic-sinusitis.
Short courses of oral steroids (clinician-directed)
- May be considered for significant swelling or polyps. Potential benefits must be balanced with side effects.
Antibiotics for bacterial exacerbations (not routine)
- Considered when there is clinical evidence suggesting an acute bacterial process. Choice of antibiotic (for example, amoxicillin-clavulanate) depends on individual factors and local resistance patterns. Repeated antibiotics without objective evidence can add risks without addressing the underlying inflammation.
Procedures when medical therapy isn’t enough
- FESS (functional endoscopic sinus surgery): Opens natural drainage pathways and removes obstructive inflammatory tissue (including polyps when present). Surgery can improve airflow and help rinses/sprays work better, but ongoing medical therapy still matters afterward.
- Balloon sinuplasty: Uses a small balloon to gently dilate certain sinus openings. It can help selected candidates based on symptoms, anatomy, and CT findings. Read more: https://sleepandsinuscenters.com/balloon-sinuplasty.
Advanced therapy for severe/uncontrolled CRS with nasal polyps (CRSwNP)
- Biologics such as dupilumab, omalizumab, and mepolizumab may be considered for selected patients with severe CRSwNP; availability and approved indications vary by region. Some other biologics may be used off-label or in research settings. In appropriate patients, biologics may improve smell, reduce polyp burden, and decrease reliance on oral steroids or revision procedures.
— Most people improve with consistent daily care and, when needed, targeted procedures or advanced therapies guided by objective findings. —

Lifestyle and Home Tips That Can Support Long-Term Relief
Lifestyle steps aren’t a cure, but they can support medical care and reduce flare frequency for some people dealing with chronic sinusitis for years.
- Use nasal rinses and sprays consistently and with proper technique. With sprays, many clinicians recommend aiming slightly outward—away from the septum.
- Reduce irritant exposure when possible (smoke/vape, heavy fragrances, harsh chemicals).
- Optimize bedroom air quality: consider dust control, appropriate humidity, and filtration if needed.
- Support sleep and hydration: hydration can help keep mucus thinner; sleep positioning may affect nighttime postnasal drip for some.
— Small, consistent habits often make a meaningful difference over time. —
When to See an ENT (and When to Seek Urgent Care)
Make an appointment if you have:
- Symptoms lasting more than 12 weeks
- Symptoms that keep returning despite OTC medications or multiple antibiotic courses
- Reduced smell lasting weeks to months
- Suspected nasal polyps or significant blockage
Red flags (urgent evaluation)
Seek urgent evaluation for:
- Swelling around the eye or vision changes
- Severe headache with high fever or stiff neck
- Confusion or neurological symptoms
- Persistent one-sided symptoms with bleeding or unexplained weight loss
— Don’t wait on red flags; seek prompt care if these symptoms occur. —
FAQs
Can chronic sinusitis last for years?
Yes. Chronic sinusitis for years can happen—especially when driven by inflammation, nasal polyps, allergies, or anatomy rather than a single infection. CRS is defined by symptoms lasting more than 12 weeks (EPOS 2020).
Why do I keep getting prescribed antibiotics if it’s chronic?
Some people have bacterial flare-ups on top of chronic inflammation. Objective evaluation (exam/endoscopy and sometimes CT) can help clarify when antibiotics are likely to help and when other treatments are more appropriate (AAO-HNSF).
What’s the best treatment for chronic sinusitis?
There isn’t one best treatment for everyone. Many evidence-based plans start with saline irrigation and intranasal corticosteroids, then add targeted therapies (like allergy management) or procedures (FESS/balloon) when needed. Biologics may be considered for severe, uncontrolled CRSwNP (EPOS 2020).
Does balloon sinuplasty work for chronic sinusitis?
It can help selected patients. Candidacy depends on the type of disease, anatomy, and CT findings. Some CRS patterns respond better than others. See: https://sleepandsinuscenters.com/balloon-sinuplasty.
What if I have chronic sinus symptoms but a normal CT?
A normal CT can suggest symptoms may be coming from rhinitis without sinus disease, migraine/TMJ, or other causes. An ENT visit can help redirect treatment toward the most likely source.
Key Takeaways (1-minute summary)
- Chronic rhinosinusitis is defined by symptoms lasting more than 12 weeks and is often inflammatory rather than purely infectious.
- The best outcomes usually come from the right diagnosis plus consistent daily care (rinses/sprays).
- Treatment options range from medical therapy to procedures like FESS or balloon sinuplasty, and biologics for severe, uncontrolled CRS with nasal polyps.
Next Step: Schedule an Evaluation
If you’ve been dealing with chronic sinusitis for years (or even just months), a focused evaluation can help clarify whether CRS is truly present and which treatments are most likely to help. Sleep and Sinus Centers of Georgia offers comprehensive sinus evaluations that may include nasal examination, nasal endoscopy, discussion of triggers (including allergies), and CT planning when appropriate.
To take the next step, book an appointment at https://www.sleepandsinuscenters.com/.
References
- Fokkens WJ, et al. EPOS 2020 Executive Summary (European Position Paper on Rhinosinusitis and Nasal Polyps). Rhinology Journal Supplement. http://rhinologyjournal.com/Documents/Supplements/EPOS2020_executive_summary.pdf
- AAO-HNSF Clinical Practice Guideline: Adult Sinusitis. https://www.entnet.org/quality-practice/quality-products/clinical-practice-guidelines/adult-sinusitis/
- Chronic rhinosinusitis overview article (PubMed Central). http://pmc.ncbi.nlm.nih.gov/articles/PMC12105074
- Endoscopic Balloon Sinuplasty policy/evidence overview. http://mo-central.medica.com/Document-Library/pdf/Medical-Policies/Endoscopic-Balloon-Sinuplasty-9667
“This article is for educational purposes only and is not medical advice. Please consult a qualified healthcare provider for diagnosis and treatment.”
Don’t let allergies slow you down. Schedule a comprehensive ENT and allergy evaluation at Sleep and Sinus Centers of Georgia. We’re here to find your triggers and guide you toward lasting relief.







