Natural Remedies vs Medical Treatment for Sinus Infections: Best Options for Fast Relief
Sinus pressure, congestion, and thick drainage can make you desperate for quick relief—so should you try home remedies, or do you need medical treatment?
Here’s the reassuring part: most sinus infections are caused by viruses and tend to improve with time and supportive care. That’s why antibiotics are not routinely recommended for uncomplicated acute sinus symptoms unless a bacterial infection is likely (IDSA, 2012). If you’ve ever wondered about natural remedies vs medical treatment for sinus infections, the best approach is usually stepwise: start with low-risk symptom care, then escalate if the pattern fits a bacterial infection—and remember that not all “natural” options are evidence-based.
In this guide, you’ll learn:
- Common symptoms (and which ones matter most)
- Causes, including viral vs bacterial sinus infection patterns and non-infectious look-alikes
- Evidence-supported natural options and OTC choices
- When medical treatment matters—and when urgent care is needed
Key Takeaway (Fast, Practical Summary)
- For many people seeking sinus infection relief fast, a strong starting point is saline irrigation plus an intranasal corticosteroid spray (both commonly used and evidence-supported for symptom relief).
- Consider discussing antibiotics with a clinician only when symptoms are severe, persistent (>10 days), or worsen after initially improving (“double worsening”)—signs that can suggest bacterial sinusitis (IDSA, 2012).
- For a deeper dive on antibiotic decision-making, see: Do I always need antibiotics for a sinus infection? https://sleepandsinuscenters.com/blog/do-i-always-need-antibiotics-for-a-sinus-infection
- This content is general education and is not a substitute for personalized medical evaluation.

What Is a Sinus Infection (Rhinosinusitis)?
Quick definition (in plain language)
A “sinus infection” is commonly used to describe swelling and irritation of the lining inside the nose and sinuses, often after a cold or allergies. The medical term rhinosinusitis simply means inflammation of the nose (“rhino”) and sinuses together.
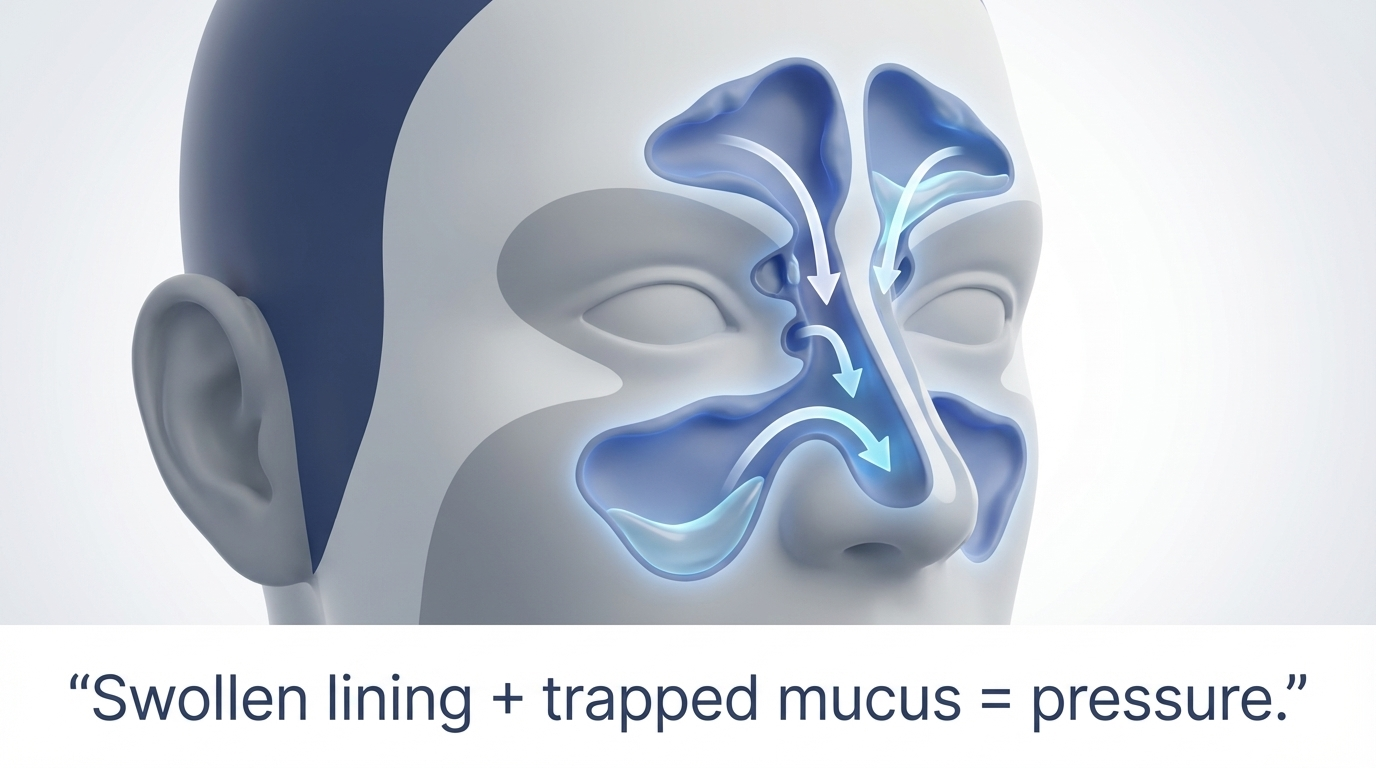
Important nuance: people often say “infection” even when the main problem is inflammation, not bacteria. A helpful way to think of it is: swollen tissues + trapped mucus = pressure and congestion, even if no bacteria are involved.
Acute vs chronic sinusitis (why it changes treatment)
- Acute rhinosinusitis: symptoms last less than 4 weeks. Most acute cases are viral and improve without antibiotics (IDSA, 2012).
- Chronic rhinosinusitis: symptoms last more than 12 weeks. Chronic cases are often more about long-term inflammation and triggers than a short-lived infection, so the strategy can be different.
This distinction matters a lot in the natural remedies vs medical treatment conversation: acute rhinosinusitis treatment often starts with supportive care, while chronic symptoms may need a longer-term plan.
Summary: Most short-term “sinus infections” are inflammatory and viral; long-lasting symptoms need a broader, long-term plan.
Sinus Infection Symptoms: What You Might Feel (and What Matters Most)
Common symptoms
Many sinus infections—viral or bacterial—can cause:
- Nasal congestion or blocked nose
- Facial pressure or fullness
- Thick nasal drainage or post-nasal drip
- Reduced smell and taste
- Cough (often worse at night)
- Fatigue, sometimes a mild fever
A common source of confusion is mucus color. Thick or colored drainage can happen in viral illness too, so it’s usually not the best “yes/no” test on its own.
Symptoms that suggest you should be more cautious
Guidelines highlight patterns that increase concern for bacterial sinusitis (IDSA, 2012), including:
- Severe symptoms (such as a high fever with significant facial pain)
- Symptoms lasting more than 10 days without improvement
- “Double worsening”: you start to feel better, then symptoms return and worsen
A clinician might summarize it like this: “We look at the timeline and intensity—how long it’s been going on and whether it’s following that classic ‘getting better, then suddenly worse’ pattern.”
Red flags—seek urgent medical care
Some symptoms can signal rare but serious complications. Seek urgent evaluation for:
- Swelling around the eyes, vision changes
- Severe headache, neck stiffness, confusion
- Severe one-sided facial swelling or rapidly worsening pain
Summary: Pay more attention to duration, severity, and double worsening than to mucus color.

Causes of Sinus Infections (and Why the Cause Determines the Best Treatment)
Viral sinus infections (most common)
Viral sinus infections often start with a regular cold. They typically improve with time and symptom support. Antibiotics don’t treat viruses, and unnecessary antibiotics can cause side effects and contribute to antibiotic resistance (IDSA, 2012).
If you’ve ever felt frustrated by being told to “wait it out,” you’re not alone. Many patients describe it as: “I don’t need a lecture—I just need to breathe.” That’s exactly where evidence-supported symptom relief can make a big difference.
Bacterial sinus infections (less common)
Bacterial sinus infections are more likely when symptoms match the guideline patterns: severe, persistent, or “double worsening” (IDSA, 2012). That’s the key to when to use antibiotics for sinus infection discussions. Only a healthcare professional can diagnose bacterial sinusitis and decide whether antibiotics are appropriate.
For a more detailed breakdown, see: Viral vs bacterial sinus infections: key differences https://sleepandsinuscenters.com/blog/viral-vs-bacterial-sinus-infections-key-differences
Non-infectious causes that mimic “sinus infection”
Not every “sinus infection” is an infection. Similar symptoms can come from:
- Allergies
- Chronic rhinitis (ongoing nasal inflammation)
- Irritants (smoke, strong fragrances)
- Structural factors (deviated septum, nasal polyps)
If symptoms keep recurring, it’s often worth asking: Is this infection—or inflammation and triggers repeating the same cycle?
Summary: The cause drives the treatment—supportive care for most viral cases; targeted care when bacterial or non-infectious factors are involved.
Natural Remedies for Fast Sinus Relief (What Helps Most—and What’s Low Risk)
Natural/home options can be great for symptom relief and drainage support, but they aren’t a substitute for evaluation when symptoms fit bacterial patterns (IDSA, 2012). Not all natural remedies are evidence-based, so focus on those with the best safety profile and supportive data.
Saline nasal irrigation (neti pot / squeeze bottle)
Saline nasal irrigation rinses out mucus and irritants, helping reduce congestion and improve nasal clearance. Think of it like a gentle “shower” for the nasal passages—mechanical cleanup that can make breathing easier. It does not treat the underlying infection (viral or bacterial), but it can meaningfully reduce symptoms and support drainage.
Safety basics matter:
- Use distilled/sterile water or water that has been boiled and cooled.
- Clean the device thoroughly and let it air-dry.
- Many people find large-volume rinses more effective than small sprays.
Evidence suggests large-volume saline (including hypertonic saline) can modestly improve symptoms, especially in chronic rhinosinusitis, though evidence quality is low-to-moderate (Cochrane, 2016; Harvey et al., 2007).
For step-by-step safety reminders, see: Neti pot safety tips https://sleepandsinuscenters.com/blog/neti-pot-safety-tips-essential-steps-for-safe-nasal-irrigation
Intranasal corticosteroid sprays (often overlooked “first-line”)
An intranasal corticosteroid spray (examples include fluticasone, budesonide, mometasone) reduces inflammation and swelling inside the nose. That can improve congestion and pressure—especially when symptoms are driven by inflammation.
Guidelines support intranasal steroids as a helpful option, and they can be more effective than saline alone for reducing symptom severity in appropriate patients (IDSA, 2012). Many people notice the biggest benefit with consistent daily use, rather than one or two sprays only when symptoms peak.
If you’re comparing spray types, this guide can help: Best nasal spray for sinusitis (steroid vs saline vs decongestant) https://sleepandsinuscenters.com/blog/best-nasal-spray-for-sinusitis-steroid-vs-saline-vs-decongestant
Humidification and steam (comfort-focused, low risk)
Humidifiers and steam can soothe irritated tissues and loosen mucus for some people. They’re popular, generally low risk, and may help comfort—though they’re not a replacement for evidence-based steps.
A practical example: a warm shower before bed can make nighttime congestion feel less intense, even if it doesn’t “cure” the underlying inflammation.
Warm compresses and hydration
- A warm compress over the face can ease pressure discomfort.
- Fluids help support normal mucus consistency (thinner mucus tends to drain more easily).
Xylitol nasal irrigation (promising but limited evidence)
A xylitol nasal rinse uses xylitol (a sugar alcohol) added to a rinse solution. Small pilot studies suggest short-term symptom improvement compared with saline alone, but evidence is still limited and needs confirmation (Weissman et al., 2011).
Natural remedies to avoid (or use cautiously)
- Undiluted essential oils inside the nose (can irritate delicate tissue)
- Overuse of certain zinc nasal products (some have been linked to smell problems depending on formulation)
- Avoid using so-called “natural antibiotics” instead of seeking medical evaluation when symptoms suggest a bacterial infection
Summary: Use low-risk options to improve comfort and drainage, but don’t let them delay professional care when warning patterns appear.

Over-the-Counter (OTC) Options: When They Help (and Common Pitfalls)
Pain and fever relief
OTC pain relievers like acetaminophen or ibuprofen can help with discomfort and fever. Always follow label directions and consider personal health conditions and medication interactions.
Decongestants (oral or spray) — short-term only
Decongestants can temporarily reduce stuffiness.
- Nasal decongestant sprays can cause rebound congestion if used for more than 3 days.
- Some people (including those with high blood pressure, heart conditions, glaucoma, thyroid disease, or pregnancy) should be cautious and check with a clinician.
If you’ve ever used a spray and felt immediate relief—then felt more blocked days later—rebound congestion may be the reason.
Antihistamines (helpful mainly if allergies are a trigger)
Antihistamines are most helpful for allergy symptoms like sneezing, itching, and watery runny nose. In some cases, they can dry secretions, which may or may not be desirable depending on symptoms.
Summary: OTC medicines can ease symptoms when used correctly and briefly, but they’re not a cure.
Medical Treatment for Sinus Infections (What Doctors Actually Recommend)
When antibiotics are appropriate (and when they aren’t)
For uncomplicated acute rhinosinusitis, antibiotics are not routinely recommended (IDSA, 2012). They’re typically considered when symptoms suggest bacterial infection:
- Severe symptoms
- Persistent symptoms >10 days without improvement
- Worsening after improving (“double worsening”) (IDSA, 2012)
Only a healthcare professional can diagnose bacterial sinusitis and determine whether antibiotics are indicated.
What “watchful waiting” means
“Watchful waiting” is a plan of symptom relief plus monitoring for improvement—or for the bacterial pattern signs above. It often includes a timeline for when to re-check or reassess.
In plain terms: “Let’s treat symptoms aggressively and smartly, but give your body time—unless the pattern changes.”
Other prescription options beyond antibiotics
- Intranasal corticosteroids may be recommended as an adjunct to reduce inflammation (IDSA, 2012).
- If allergies are suspected, a targeted allergy plan may help reduce repeat flare-ups.
When imaging or specialist evaluation is needed
- Recurrent infections
- Suspected chronic sinusitis
- Symptoms not responding to appropriate first steps, or concern for complications
Summary: Only a clinician can confirm bacterial sinusitis and tailor treatment; many acute cases improve without antibiotics.

Natural Remedies vs Medical Treatment — A Clear “What to Do First” Plan
Day 1–3: First-line home and OTC support
- Saline irrigation
- Intranasal corticosteroid spray (when appropriate)
- Humidification/steam, hydration, rest
- OTC pain relief as needed
Day 4–10: Reassess your symptom pattern
- Improving: supportive care may be enough
- Not improving: consider checking in with a clinician—especially if symptoms are significant or you have health risk factors
After 10 days (or sooner if severe): when medical care is the better option
If symptoms meet the IDSA criteria (severe, persistent >10 days, or double worsening), medical evaluation is more likely to change the plan (IDSA, 2012).
Quick comparison (evidence, risks, when to use)
Saline nasal irrigation (Cochrane 2016; Harvey 2007)
- Best for: congestion, thick mucus, post-nasal drip
- Evidence: moderate (stronger in chronic rhinosinusitis)
- Risks: water safety/device hygiene issues if done incorrectly
- When to use: early support; also helpful in chronic symptoms
Intranasal corticosteroid spray (IDSA 2012)
- Best for: inflammation-driven congestion/pressure
- Evidence: moderate
- Risks: local irritation/nosebleeds in some
- When to use: often a first-line adjunct for symptom control
Steam/humidification
- Best for: comfort, dryness
- Evidence: limited
- Risks: burns if too hot; too much humidity can worsen indoor mold
- When to use: comfort add-on
Xylitol rinse (Weissman 2011)
- Best for: added symptom support
- Evidence: limited (small studies)
- Risks: irritation in some
- When to use: optional; consider if saline alone isn’t enough
Antibiotics (IDSA 2012)
- Best for: likely bacterial sinusitis (diagnosed by a clinician)
- Evidence: strong when criteria met
- Risks: side effects, resistance
- When to use: severe/persistent/double-worsening patterns
Summary: Start simple, reassess at set intervals, and escalate only when the pattern indicates bacterial sinusitis.
Lifestyle Tips to Prevent Sinus Infections (and Speed Recovery)
Reduce triggers and improve nasal health
- Manage allergies proactively (especially if seasonal symptoms are predictable).
- Avoid smoke and strong fragrance irritants.
- Aim for balanced indoor humidity (not overly dry or damp).
Hygiene and exposure basics
- Handwashing during cold/flu season.
- Don’t share irrigation devices; clean them thoroughly.
Sleep and positioning
- Slight head elevation may help with nighttime post-nasal drip for some people.
Summary: Controlling triggers and supporting nasal health can reduce flares and help you recover faster.
FAQs (Patient-Friendly, SEO-Targeted)
How can I get rid of a sinus infection fast?
The fastest path usually means focusing on symptom control and drainage early (saline irrigation, inflammation control with an intranasal steroid when appropriate, comfort measures), then reassessing based on the time course and severity (IDSA, 2012).
Do I need antibiotics for a sinus infection?
Most people don’t. Antibiotics are usually reserved for symptoms that are severe, last more than 10 days without improvement, or worsen after improving (IDSA, 2012). Only a clinician can diagnose bacterial sinusitis.
How do I know if it’s viral or bacterial?
The most helpful clues are duration, severity, and the double-worsening pattern (IDSA, 2012). More here: Viral vs bacterial sinus infections: key differences https://sleepandsinuscenters.com/blog/viral-vs-bacterial-sinus-infections-key-differences
Is saline irrigation actually effective?
Studies suggest modest symptom improvement, particularly in chronic rhinosinusitis, and it’s generally low risk when done safely (Cochrane, 2016; Harvey et al., 2007).
Is xylitol nasal rinse better than saline?
A xylitol nasal rinse has early evidence of short-term improvement over saline, but studies are small and more research is needed (Weissman et al., 2011).
What nasal spray works best for sinusitis?
It depends on the goal:
- Steroid sprays reduce inflammation (IDSA, 2012)
- Saline rinses/sprays help wash out mucus and irritants
- Decongestant sprays shrink swelling briefly but can cause rebound if overused
More detail: Best nasal spray for sinusitis (steroid vs saline vs decongestant) https://sleepandsinuscenters.com/blog/best-nasal-spray-for-sinusitis-steroid-vs-saline-vs-decongestant
When should I see an ENT for sinus infections?
Consider evaluation if symptoms are recurrent, chronic (>12 weeks), unusually severe, or not improving with appropriate first steps—or if red flags occur.
Conclusion + Next Step
When weighing natural remedies vs medical treatment for sinus infections, the best strategy is usually staged: start with low-risk, evidence-supported symptom relief (especially saline irrigation and an intranasal corticosteroid spray when appropriate), and avoid unnecessary antibiotics. If symptoms become severe, last beyond 10 days, or follow a “double worsening” pattern, evaluation may be more likely to change treatment (IDSA, 2012).
If you’d like help sorting out your symptom pattern—especially if you’re dealing with repeat episodes or lingering congestion—Sleep and Sinus Centers of Georgia can help you plan next steps and understand your options. To book an appointment, visit https://www.sleepandsinuscenters.com/. You can also explore: Do I always need antibiotics for a sinus infection? https://sleepandsinuscenters.com/blog/do-i-always-need-antibiotics-for-a-sinus-infection
Sources
- Infectious Diseases Society of America (IDSA). (2012). Clinical Practice Guideline for Acute Bacterial Rhinosinusitis in Children and Adults. https://www.idsociety.org/practice-guideline/rhinosinusitis/
- Schilder, A. G. M., Chong, L. Y., et al. (2016). Saline irrigation for chronic rhinosinusitis (Cochrane Review). https://discovery.ucl.ac.uk/1489911/1/Schilder_Chong_et_al-2016-The_Cochrane_library.pdf
- Harvey, R. J., et al. (2007). Saline irrigation in chronic rhinosinusitis. https://pubmed.ncbi.nlm.nih.gov/17636843/
- Weissman, J. D., et al. (2011). Xylitol nasal irrigation pilot RCT. https://pubmed.ncbi.nlm.nih.gov/21994147/
Disclaimer
This article is for educational purposes only and is not medical advice. Please consult a qualified healthcare provider for diagnosis and treatment.
Don’t let allergies slow you down. Schedule a comprehensive ENT and allergy evaluation at Sleep and Sinus Centers of Georgia. We’re here to find your triggers and guide you toward lasting relief.








