Broken Sinus: Symptoms, CT Diagnosis & Treatment
Facial injuries can be confusing—especially when you hear a term like “broken sinus.” In everyday language, this usually refers to a fracture of the bones that form the walls of the paranasal sinuses (frontal, maxillary, ethmoid, or sphenoid) and sometimes nearby orbital bones around the eye. “Broken sinus” is not a formal medical diagnosis; clinicians typically document a paranasal sinus fracture or fracture of a specific sinus wall. These injuries are often evaluated with CT imaging to identify and characterize the fracture and check for complications.
A helpful way to picture it: your sinuses are like air-filled rooms, and the facial bones are the walls and ceilings. Trauma can crack those walls—even if your nose looks “fine” from the outside.
Why does it matter? Beyond pain and swelling, a sinus fracture can occasionally affect vision, normal sinus drainage, or—in more serious cases—cause a CSF leak (cerebrospinal fluid), which increases infection risk. Many uncomplicated, nondisplaced fractures can heal without surgery, but certain “red flag” symptoms call for urgent evaluation.
Medical disclaimer: This article is for general education and is not a substitute for medical care. Seek urgent evaluation for red-flag symptoms, especially after facial trauma.
What Counts as a “Broken Sinus”? (Anatomy + common fracture locations)
A sinus fracture (paranasal sinus fracture) involves one or more of the bony walls surrounding these spaces.
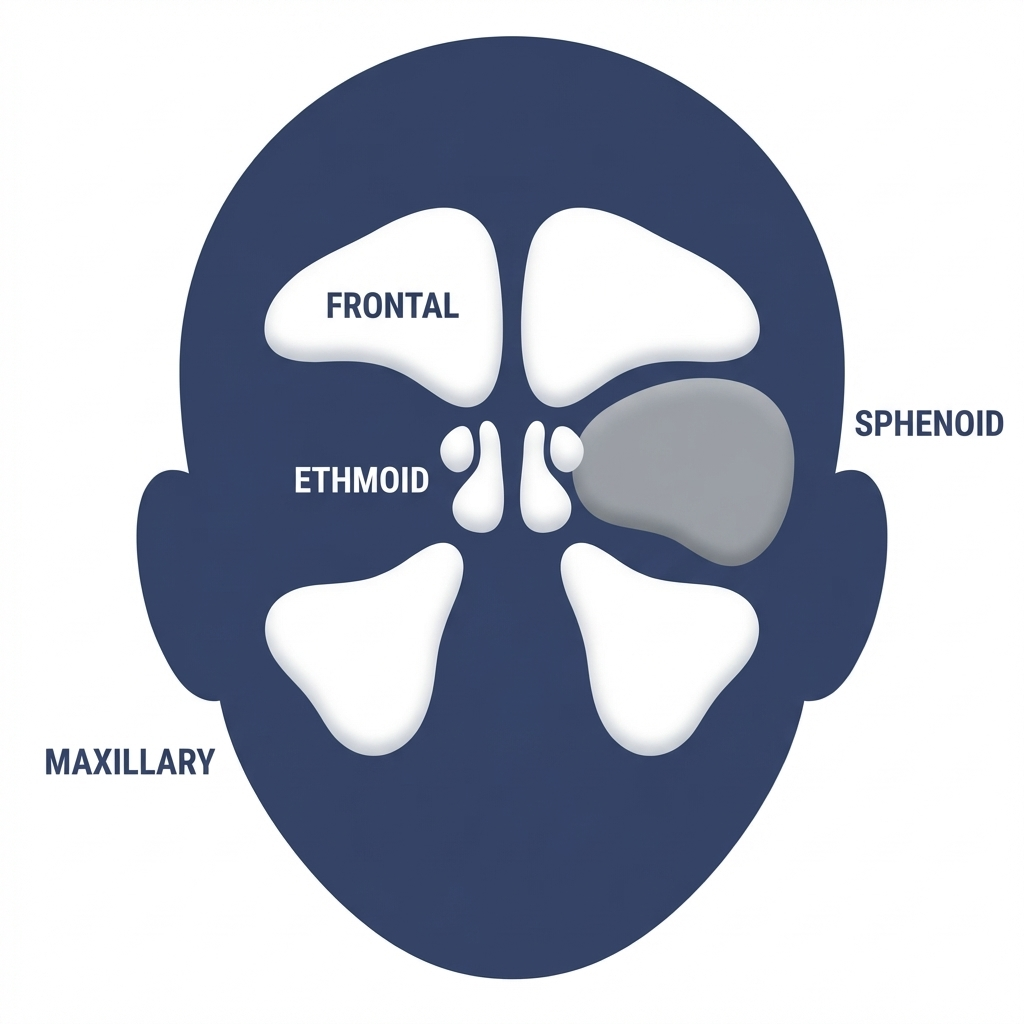
The four paranasal sinuses (simple map for patients)
- Frontal sinuses: in the forehead
- Maxillary sinuses: in the cheeks (under the eyes)
- Ethmoid sinuses: between the eyes
- Sphenoid sinuses: deeper behind the nose
— In short, a “broken sinus” usually means a fracture of the bony sinus walls, not the air space itself. —
Why sinus fractures can feel “indirect”
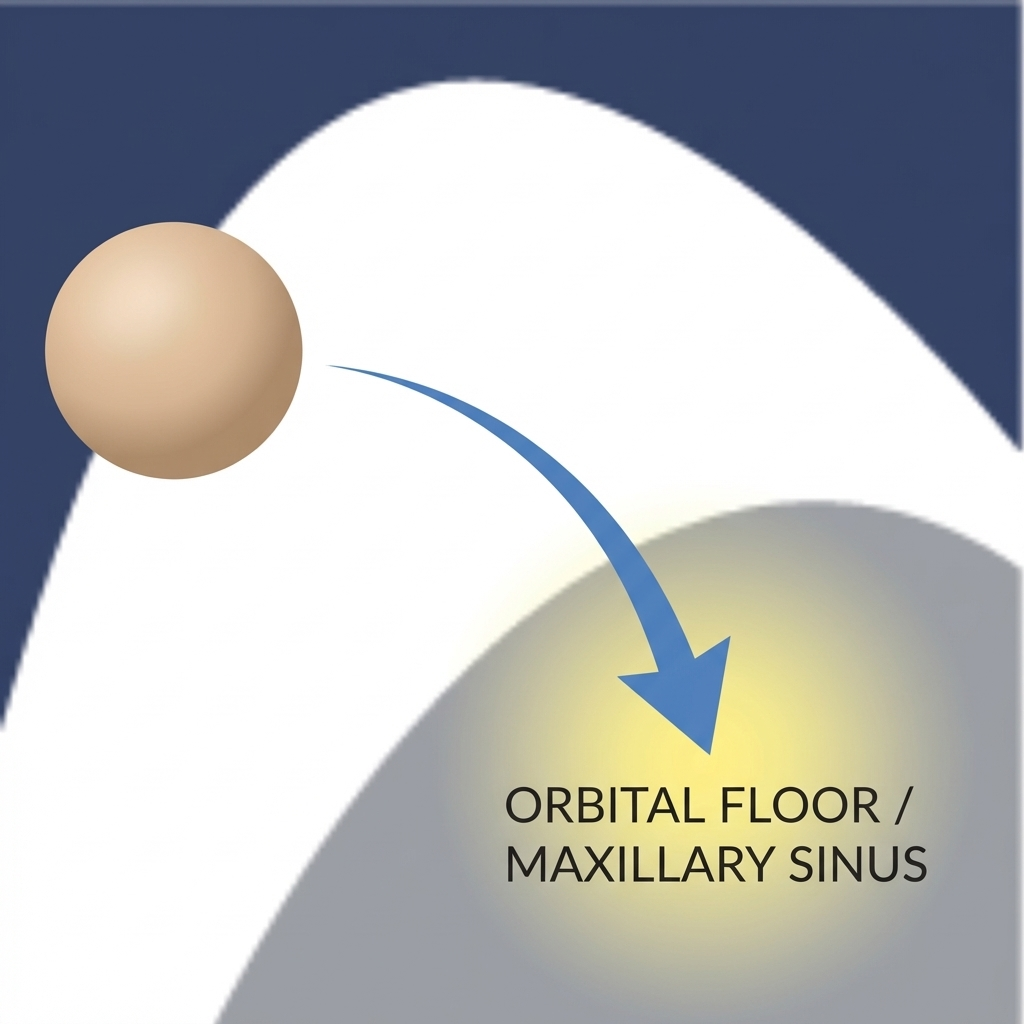
You don’t always need a direct hit to the nose to injure a sinus wall. For example, a hard impact to the cheek can transmit force into the maxillary sinus or the orbital floor. The orbital floor forms the roof of the maxillary sinus, so injuries can involve both areas. This is one reason clinicians rely on imaging rather than appearance alone.
Common patterns doctors see
- Frontal sinus fracture: can carry a higher risk of complications depending on which wall is involved.
- Maxillary sinus fracture: often involves the front wall of the sinus after a direct blow to the cheek.
- Orbital floor fracture: can co-occur with maxillary sinus wall injury because of their close anatomic relationship.
Because these areas connect anatomically, a broken sinus may occur with an orbital floor fracture or other facial fractures even if the nose appears relatively normal. Diagnosis requires clinical evaluation and imaging to confirm the exact injury pattern.
Causes and Risk Factors (How sinus fractures happen)
Most common causes
Sinus and orbital fractures most often happen due to blunt facial trauma, such as:
- Sports injuries (balls, elbows, collisions)
- Falls (especially onto the face)
- Motor vehicle accidents (often higher-energy)
- Assault or being struck in the face
Who is at higher risk for complications
Complication risk tends to be higher with:
- High-force injuries or multiple injuries at once (polytrauma)
- Prior facial trauma or surgery that changes anatomy
- Symptoms that suggest orbital involvement (eye symptoms) or skull base involvement (possible CSF leak)
If the injury involves the frontal sinus—especially the deeper wall (posterior table)—clinicians generally take it more cautiously due to the proximity to the brain and infection risk.
— Bottom line: most sinus wall fractures follow blunt facial trauma, with higher risk in high‑energy injuries. —
Symptoms of a Broken Sinus (What patients may notice)
Common symptoms (may start immediately)
- Facial pain/pressure (forehead or cheek)
- Swelling, bruising, tenderness
- Nasal congestion or stuffiness
- Nosebleeds
- Headache
It’s normal for early symptoms to overlap with bruising and soft-tissue injury. Concern increases with symptom progression, location (forehead vs cheek), and the presence of eye symptoms or unusual drainage. These symptoms can also overlap with other facial injuries. For related information, see nasal fracture symptoms: https://sleepandsinuscenters.com/blog/nasal-fracture-symptoms-and-care-key-signs-and-treatment-tips
Signs that suggest sinus/orbital involvement (higher suspicion)
- Subcutaneous emphysema: a crackling sensation under the skin from trapped air
- Numbness/tingling of the cheek/upper lip: can reflect infraorbital nerve irritation
- Double vision (diplopia) or pain with eye movement

Red-flag symptoms (seek urgent/emergency care)
- Clear watery drainage from the nose after trauma (clear rhinorrhea) that may indicate a CSF leak
- Worsening vision, severe eye pain, or a bulging eye
- Confusion, severe headache, fever, or neck stiffness (possible intracranial or infectious complications)
- An eye that can’t move normally or seems “stuck” (possible muscle entrapment)
If you’re unsure whether drainage is “just a runny nose,” the context matters: new, persistent, watery clear drainage after trauma is a reason to be evaluated urgently.
— If eye symptoms or clear, one‑sided watery drainage appear, treat them as red flags after facial trauma. —
How Doctors Diagnose a Broken Sinus
History + physical exam (what clinicians check)
Evaluation usually begins with the details of the injury and a careful exam, which may include:
- How the injury happened (force, direction, object involved)
- Facial symmetry and tenderness
- Checking for “step-offs” (areas where bone alignment feels irregular)
- A basic eye assessment (vision clarity, pupils, eye movements, double vision)
- Nasal exam for bleeding, swelling, and concerning findings such as septal hematoma

Imaging—CT is usually the best test
For suspected sinus fracture injuries, a CT scan is generally the imaging test of choice because it shows facial bones in high detail and helps evaluate fracture location, displacement, and possible complications.
A CT scan for sinus fracture evaluation can show, in plain language:
- Hemosinus: blood in a sinus (often seen as an air–fluid level)
- Which bony wall is fractured and whether it is displaced
- Whether sinus drainage pathways look disrupted
- Orbital floor fracture defects and possible soft-tissue entrapment
Related reading: CT scan for a sinus fracture https://sleepandsinuscenters.com/blog/sinus-ct-scan-what-it-shows-and-how-it-helps-diagnose-sinus-issues
CBCT vs CT (why your doctor may choose one)
In selected situations, cone-beam CT (CBCT) can detect certain fractures (including some anterior maxillary wall fractures). However, for broader trauma evaluation—or when skull base or intracranial injury is a concern—standard CT is generally preferred.
— Definitive diagnosis typically relies on CT to localize and characterize fractures and related complications. —
Treatment Options for a Broken Sinus (Observation vs surgery)
Management depends on which sinus wall is involved, how displaced the fracture is, and whether complications exist. Many recommendations come from expert reviews and case series rather than large head-to-head trials.

What “observation” usually means (so it doesn’t feel like “doing nothing”)
When clinicians recommend non-surgical care, it typically includes a plan: symptom control, activity precautions, and follow-up to ensure the fracture heals and the sinus continues to drain normally.
When observation (non-surgical management) may be enough
- No CSF leak
- No vision problems or muscle entrapment
- No clear blockage of sinus drainage pathways
Indications for urgent or surgical repair
Surgery is more likely to be discussed when fractures create functional risk, such as:
- CSF leak concerns (clear rhinorrhea), or suspected deeper frontal sinus involvement
- Eye-threatening issues include:
- Muscle entrapment
- Progressive visual loss
- Retrobulbar hemorrhage
- Significant change in eye position (enophthalmos), with specific thresholds used in surgical planning
- Fractures that appear to block sinus drainage, which can raise the risk of chronic infection or mucocele formation (especially in the frontal sinus)
Frontal sinus fractures deserve special attention
A frontal sinus fracture may need closer monitoring because it can be associated with complications such as:
- CSF leak
- Meningitis
- Mucocele
- Osteomyelitis
Care is often multidisciplinary depending on the injury pattern (ENT, ophthalmology, and sometimes neurosurgery involvement). Antibiotic use is individualized and varies by injury pattern and specialist guidance; it is not routine in all cases.
Medications and supportive care (what may be used)
- Pain relievers
- Antibiotics in selected situations (for example, open fractures or higher-risk frontal sinus injuries, based on specialist guidance)
- Individualized nasal care precautions (for example, early guidance about nose blowing)
For comparison with nasal injury care, see broken nose treatment: https://sleepandsinuscenters.com/blog/broken-nose-treatment-when-to-see-an-ent-specialist
— Treatment ranges from careful observation to surgery, guided by CT findings and function‑threatening signs. —
Recovery and At-Home Care (Lifestyle tips)
Healing time and restrictions vary depending on fracture location (maxillary vs frontal), whether the orbit is involved, and whether surgery was needed. In general, clinicians often emphasize:
Do’s (help healing and reduce complications)
- Cold packs early and head elevation for swelling
- Keeping follow-up appointments (some complications can appear later)
- Monitoring for new or worsening symptoms (vision changes, fever, increasing pain, new drainage)
Don’ts (common precautions after suspected sinus fracture)
- Avoid forceful nose blowing
- Avoid heavy lifting/straining until cleared
- Avoid contact sports until approved
When can you return to work/sports?
Return-to-activity decisions are individualized. Fractures involving the orbit or frontal sinus often require more cautious timelines and follow-up due to higher complication risk. If you’re eager to return to training or a physical job, ask your clinician for clear guidance based on your CT findings.
— Follow precautions and keep follow‑up, since some complications emerge days to weeks after injury. —
Possible Complications (Why follow-up matters)
Sinus-related complications
- Chronic sinusitis due to drainage obstruction
- Mucocele formation (notably associated with frontal sinus injuries)
- Recurrent infection
Eye and nerve complications
- Persistent double vision or eye position changes (enophthalmos)
- Persistent numbness in the cheek/upper lip region
Intracranial/infectious risks (more likely with frontal sinus/posterior wall)
- CSF leak can increase the risk of meningitis, which is why clear rhinorrhea after trauma is treated as a warning sign.
— Timely evaluation and follow‑up reduce the risk of sinus, eye, and intracranial complications. —
Frequently Asked Questions (FAQ)
Can a sinus be “broken” without a broken nose? Yes. The sinus walls and orbital bones can fracture even when the nasal bones aren’t clearly broken on the outside. Imaging and clinical evaluation are needed to confirm the diagnosis. For comparison, see broken nose treatment: https://sleepandsinuscenters.com/blog/broken-nose-treatment-when-to-see-an-ent-specialist
How do I know if clear runny nose fluid is CSF? After facial trauma, watery, persistent (often one-sided) clear rhinorrhea can be concerning for CSF leak and deserves urgent medical evaluation.
What imaging do I need—X-ray or CT? For suspected paranasal sinus fracture injuries, CT is typically preferred because it defines fracture location, displacement, and possible complications more accurately.
Do all broken sinuses need surgery? No. Many uncomplicated, nondisplaced fractures with no drainage issues, CSF leak, or vision problems can be managed without surgery.
Why are frontal sinus fractures treated more cautiously? A frontal sinus fracture can be associated with more serious complications (including CSF leak, meningitis, and mucocele), so closer follow-up and sometimes surgical planning are more common.
How long does it take to heal? Timelines vary widely based on severity and location. Many uncomplicated facial fractures improve over weeks, but follow-up matters because some issues (like chronic drainage problems) may show up later.
When to See an ENT or Go to the ER (Clear callouts)
Go to the ER now if you have:
- Vision changes, severe eye pain, or a bulging eye
- Clear watery drainage after facial trauma (possible CSF leak)
- Confusion, severe headache, fever, or neck stiffness
Schedule urgent ENT/facial trauma evaluation if:
- Persistent facial numbness or worsening swelling/pain
- Ongoing nosebleeds or suspected fracture after an impact
- Double vision or new difficulty moving the eye
If you’re unsure about the next step after facial trauma, this guide on when to see an ENT can help: https://sleepandsinuscenters.com/blog/when-should-i-see-an-ent
Need help reviewing symptoms or next steps? Book an appointment with an ENT at Sleep & Sinus Centers: https://www.sleepandsinuscenters.com/
— When in doubt after facial trauma, err on the side of urgent assessment. —
Conclusion
A “broken sinus” usually refers to a facial fracture involving the paranasal sinuses and sometimes the orbit. Because symptoms can range from mild swelling to serious red flags like CSF leak or vision problems, evaluation often includes a CT scan to confirm the diagnosis and assess for complications. Treatment ranges from observation to surgical repair, especially when sinus drainage pathways, the orbit, or the frontal sinus are involved.
References
1. StatPearls. Orbital Floor Fracture (2023). NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK534825/
2. Radiopaedia. Paranasal sinus fractures. https://radiopaedia.org/articles/paranasal-sinus-fractures?lang=us
3. Metzinger SE, Metzinger RC. Complications of Frontal Sinus Fractures (2009). Facial Plast Surg. https://pmc.ncbi.nlm.nih.gov/articles/PMC3052648/
4. Yilmaz SY, et al. Diagnosis of Maxillary Sinus Fracture with Cone-Beam CT (2014). https://pmc.ncbi.nlm.nih.gov/articles/PMC4078170/
5. Facial Trauma MD. Sinus Fracture. https://facialtraumamd.com/sinus-fracture/
This article is for educational purposes only and is not medical advice. Please consult a qualified healthcare provider for diagnosis and treatment.
Don’t let allergies slow you down. Schedule a comprehensive ENT and allergy evaluation at Sleep and Sinus Centers of Georgia. We’re here to find your triggers and guide you toward lasting relief.








