Granulomatosis With Polyangiitis (GPA): Chronic Sinus Symptoms, Causes, and Treatment
Persistent “sinus infections” can be frustrating—especially when congestion, pressure, and drainage keep returning or don’t improve as expected. Most of the time, chronic sinus symptoms are caused by common problems like inflammation, allergies, or recurrent infections. But in a small number of people, Granulomatosis with Polyangiitis (GPA) chronic sinus symptoms can look very similar to routine sinusitis at first, which may delay the right diagnosis.
This article is educational and patient-focused: what GPA is, how it can affect the nose and sinuses, what makes it different from typical chronic sinusitis, how it’s diagnosed, and what treatment generally involves.
Medical disclaimer: This content is for education only and is not a substitute for personalized medical advice, diagnosis, or treatment. If you have worsening symptoms, significant bleeding, breathing issues, or concern for systemic illness, seek prompt medical care.
Quick Take—Why GPA Can Look Like “Just a Sinus Infection”
Granulomatosis with polyangiitis (GPA) is a rare autoimmune disease that causes inflammation in small blood vessels (a form of vasculitis). It commonly involves the nose/sinuses and lungs, and it can also affect the kidneys. Because it often starts with upper-airway symptoms, early Granulomatosis with Polyangiitis (GPA) chronic sinus symptoms may mimic a cold, allergies, or a routine sinus infection.
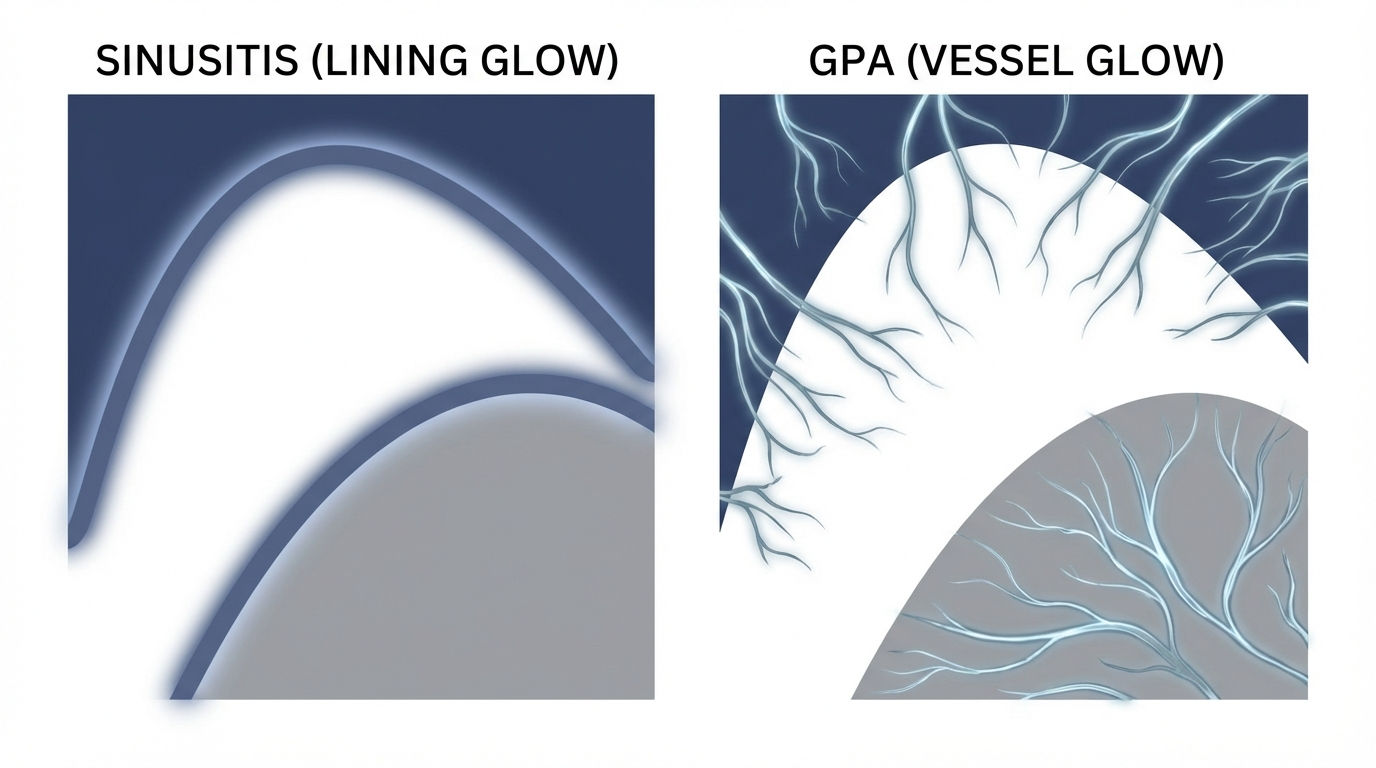
A helpful way to think about it: typical sinusitis is often “inflammation in the lining,” while GPA can be “inflammation in the blood vessels feeding that lining,” which may create a different pattern over time. Persistent or unusual symptoms that don’t improve with standard treatment deserve a closer look. Sources: Mayo Clinic, Cleveland Clinic, Johns Hopkins Medicine.
If you’re trying to sort out whether your symptoms fit a typical pattern, you may also find it helpful to review our overview of chronic sinusitis: https://sleepandsinuscenters.com/chronic-sinusitis
Summary: Persistent congestion plus crusting or nosebleeds that don’t respond to usual care should prompt a closer look for autoimmune causes like GPA.
What Is Granulomatosis With Polyangiitis (GPA)?
GPA (formerly Wegener’s granulomatosis) is an autoimmune condition where the immune system mistakenly attacks the body’s small blood vessels. That inflammation can reduce healthy blood flow and injure nearby tissues—especially in the airways.
The areas most commonly involved include: upper airway (nose and sinuses); lower airway (lungs); kidneys. Sources: Mayo Clinic; Cleveland Clinic.
Where ENT symptoms fit in GPA
ENT (ear, nose, and throat) symptoms often appear early in GPA. A common real-world scenario is someone treated multiple times for “sinus infections,” briefly feeling better, then flaring again—especially when symptoms include prominent crusting or bleeding, not just congestion. Because of this, ENT evaluation can play an important role in recognizing patterns that suggest an autoimmune cause. Source: Johns Hopkins Medicine.
Summary: GPA often begins with nose and sinus symptoms, so ENT evaluation can be key to early recognition.
Chronic Sinus & Nasal Symptoms of GPA (What Patients Notice)
Common early symptoms that mimic a cold or sinus infection: persistent nasal congestion/stuffiness; sinus pressure or facial pain; thick or pus-like nasal drainage; nasal crusting/scabbing; nasal sores/irritation; frequent or recurrent nosebleeds (crusting + nosebleeds together can be an important clue). Sources: Mayo Clinic; Cleveland Clinic; Johns Hopkins Medicine.
What this can feel like day-to-day: congestion that never quite clears; painful dryness inside the nose; crusts that return soon after cleaning; nosebleeds that seem “too easy” (for example, after gentle blowing or rinsing). These aren’t diagnostic on their own—but they can be meaningful in context.
More severe sinonasal problems (often later or during active disease): tissue damage and ulcers in the nose; septal perforation (a hole in the nasal septum); changes in nasal shape such as saddle nose deformity; more destructive changes inside the nasal cavity (including turbinate injury). These changes are not the typical course for routine sinusitis and raise concern for an underlying inflammatory or autoimmune process. Sources: ScienceDirect review (2024); PMC review on ENT involvement.
Can sinus symptoms be the only sign of GPA? Yes. In some people, sinonasal symptoms may be the primary or even the only presenting feature for a time, which can lead to misdiagnosis as “recurrent infection,” especially if symptoms temporarily improve and then flare again. Sources: ScienceDirect review (2024); PMC review.
Summary: When crusting, bleeding, or tissue injury accompany “sinus infections,” GPA should be on the radar.

GPA vs “Regular” Chronic Sinusitis—Clues Something Else Is Going On
Red flags for autoimmune-related sinus disease (not diagnostic on their own): symptoms that persist despite antibiotics and standard sinus care; frequent nosebleeds plus heavy crusting/scabbing; painful nasal sores/ulcers; a new whistling sound when breathing through the nose (possible septal perforation); unexplained fatigue, fevers, or weight loss; new cough, shortness of breath, or coughing up blood; urinary changes (like blood in urine) or new swelling—these can suggest kidney involvement and should be evaluated promptly. Sources: Cleveland Clinic; Mayo Clinic; Cleveland Clinic ConsultQD.
If you want a broader view of non-infectious causes, see: https://sleepandsinuscenters.com/blog/autoimmune-sinusitis-key-signs-your-sinus-problems-20260203051202
Why it’s commonly mistaken for infection or allergies: overlap with viral URIs, bacterial sinusitis, and allergic rhinitis; GPA may cycle between flares and remissions, adding to early confusion. Sources: Johns Hopkins Medicine; Mayo Clinic.
Summary: If sinus symptoms cycle and resist usual treatments—especially with crusting/bleeding—ask about autoimmune causes.
What Causes GPA? (And What Doesn’t)
The underlying mechanism: autoimmune small-vessel vasculitis. When blood vessels become inflamed, nearby tissue can be irritated or damaged due to reduced blood flow and ongoing immune activity. In the nose and sinuses, that can contribute to chronic inflammation, crusting, and sometimes tissue injury. Sources: Mayo Clinic; Cleveland Clinic.
ANCA and GPA (simple view): GPA is often grouped under ANCA-associated vasculitis. ANCA blood tests can be positive in many with GPA, but not all. A negative ANCA does not rule out GPA; diagnosis requires clinical correlation with symptoms, imaging, and sometimes biopsy. Source: Everyday Health.
Is GPA contagious? Is it caused by a virus? GPA is not contagious. The exact cause isn’t fully understood; it’s considered an autoimmune condition with triggers that vary between individuals. Source: Mayo Clinic.
Summary: GPA is autoimmune, not contagious—and ANCA helps but doesn’t make or break the diagnosis by itself.

How Doctors Diagnose GPA When Sinus Symptoms Won’t Quit
Medical history + ENT exam typically review: duration and changes in symptoms; response (or lack of response) to antibiotics/steroids; patterns of crusting and nosebleeds; symptoms outside the sinuses (lungs, kidneys, general symptoms). ENT evaluation may include nasal endoscopy for a detailed look at inflammation, crusting, bleeding, or ulcers.
Testing that may be ordered: blood tests (inflammation markers and possibly ANCA); imaging (CT sinuses; chest imaging if respiratory symptoms); urine tests and kidney function tests; biopsy in select cases to confirm vasculitis and granulomatous inflammation. Sources: Mayo Clinic; Johns Hopkins Medicine; Cureus (diagnostic pitfalls).
Why early diagnosis matters: GPA can involve lungs and kidneys; earlier identification helps reduce the risk of serious complications and guides treatment. Sources: Cleveland Clinic; Mayo Clinic.
Summary: Diagnosis blends symptoms, exam, labs, imaging, and sometimes biopsy—no single test tells the whole story.

Treatment Options for GPA (Systemic + Sinus-Focused Care)
Treatment is individualized and commonly coordinated by rheumatology, with support from ENT and other specialists depending on which organs are involved.
The big picture: two phases—induction therapy to calm active inflammation quickly; maintenance therapy to keep disease controlled and reduce relapse risk. Sources: Cleveland Clinic; Mayo Clinic.
Medications commonly used (high-level): corticosteroids (often early); immune-targeting therapies for vasculitis (for example, rituximab or cyclophosphamide for induction; methotrexate, azathioprine, or mycophenolate for maintenance); ongoing monitoring for side effects and infection risk. Sources: Mayo Clinic; Cleveland Clinic.
ENT treatments that may help chronic sinus symptoms (supportive care): saline irrigations; topical therapies such as nasal steroid sprays/rinses when appropriate; humidification and strategies to reduce bleeding/irritation; treating secondary bacterial infections when confirmed—avoiding routine/repeated antibiotics when infection is unlikely. Sources: PMC review; Sleep and Sinus Centers of Georgia overview.
When surgery might be discussed: sometimes for obstruction or complications, but it does not treat the underlying autoimmune disease; medical control of inflammation guides timing and planning. Source: PMC review.
Summary: GPA care targets the immune system first; ENT treatments support comfort and function, and antibiotics are used only when infection is likely.

Lifestyle & Self-Care Tips for GPA-Related Nasal/Sinus Symptoms (Adjuncts)
Gentle daily routines that may reduce irritation: use a humidifier and clean it properly; for saline rinses, use sterile/distilled water (or boiled and cooled) per product instructions; avoid picking crusts—soften first; avoid smoke, strong fragrances, and other irritants when possible. Self-care supports comfort but doesn’t replace medical treatment when GPA is suspected or confirmed.
Track symptoms like a clinician: frequency/severity of nosebleeds; amount of crusting and congestion; facial pain/pressure patterns; fevers, fatigue, or weight changes; any new cough or shortness of breath; medication changes and responses. Dated photos of visible changes can help your clinician see patterns over time.
Summary: Supportive routines help comfort, but medical therapy is essential if GPA is driving symptoms.
FAQs (Patient-Friendly)
Is GPA the same thing as chronic sinusitis? No—GPA is a systemic vasculitis that can cause chronic sinus symptoms, but it isn’t the same as routine chronic sinusitis. Sources: Mayo Clinic; Cleveland Clinic.
Why do I keep getting “sinus infections” that don’t go away? Ongoing symptoms can come from chronic inflammation, allergies, anatomy, recurrent infections, or (less commonly) autoimmune inflammation like GPA. Persistent, unusual patterns deserve evaluation. Sources: ScienceDirect (2024); Sleep and Sinus Centers of Georgia overview.
What does nasal crusting mean in GPA? Crusting can result from inflamed or damaged nasal lining and may be persistent in GPA, sometimes with bleeding or sores. Sources: Cleveland Clinic; PMC review.
Can GPA cause a hole in the septum or change the shape of the nose? Yes—more destructive sinonasal disease can lead to septal perforation or saddle nose deformity. Sources: ScienceDirect (2024); PMC review.
Which doctor treats GPA? Systemic treatment is often led by rheumatology; ENT manages nasal and sinus complications. Pulmonology and nephrology may be involved if lungs or kidneys are affected. Sources: Cleveland Clinic; Johns Hopkins Medicine.
When to Seek Urgent Care vs Scheduling an ENT Visit
Seek urgent/emergency care for: heavy or uncontrolled nosebleeds; shortness of breath, chest pain, or coughing blood; severe weakness, fainting, or confusion; signs suggesting significant kidney issues (markedly decreased urination or swelling). Sources: Mayo Clinic; Cleveland Clinic.
Make an appointment when: sinus symptoms last for weeks, keep returning, or don’t respond as expected; ongoing crusting plus nosebleeds plus facial pain; symptoms are unusual or worsening. Practical guidance: https://sleepandsinuscenters.com/blog/when-should-i-see-an-ent
Summary: Seek urgent care for severe or systemic warning signs; schedule an ENT visit when symptoms persist or don’t follow the usual pattern.
Conclusion + Next Step
Most sinus problems are not GPA. Still, when Granulomatosis with Polyangiitis (GPA) chronic sinus symptoms are present, they can masquerade as routine sinusitis—especially early on. Persistent congestion with prominent crusting, recurrent nosebleeds, or symptoms that don’t improve as expected may warrant a more thorough evaluation.
If you’re dealing with ongoing sinus symptoms that don’t follow the typical “infection/allergy” pattern, consider scheduling an ENT evaluation. Book an appointment with Sleep and Sinus Centers of Georgia: https://www.sleepandsinuscenters.com/
To keep learning: autoimmune sinusitis overview: https://sleepandsinuscenters.com/blog/autoimmune-sinusitis-key-signs-your-sinus-problems-20260203051202; chronic sinusitis page: https://sleepandsinuscenters.com/chronic-sinusitis; “When should I see an ENT?”: https://sleepandsinuscenters.com/blog/when-should-i-see-an-ent
Summary: Most sinus issues aren’t GPA, but persistent, atypical symptoms deserve a careful, coordinated evaluation.
Sources
Mayo Clinic – GPA overview and symptoms/causes: https://www.mayoclinic.org/diseases-conditions/granulomatosis-with-polyangiitis/symptoms-causes/syc-20351088
Cleveland Clinic – GPA overview: https://my.clevelandclinic.org/health/diseases/granulomatosis-with-polyangiitis-formerly-wegeners-granulomatosis
Johns Hopkins Medicine – Wegener’s granulomatosis: https://www.hopkinsmedicine.org/health/conditions-and-diseases/wegeners-granulomatosis
ScienceDirect (2024) – Sinonasal manifestations review: https://www.sciencedirect.com/science/article/pii/S0385814624000415
PMC – ENT involvement review: https://pmc.ncbi.nlm.nih.gov/articles/PMC10276886/
Cleveland Clinic ConsultQD – case discussion: https://consultqd.clevelandclinic.org/case-report-granulomatosis-with-polyangiitis-and-persistent-shortness-of-breath
Everyday Health – ANCA vasculitis subtypes: https://www.everydayhealth.com/autoimmune-diseases/gpa-mpa-egpa-guide-to-anca-vasculitis-subtypes/
Cureus (PDF) – diagnostic pitfalls: https://www.cureus.com/articles/448830-beyond-infection-and-malignancy-diagnostic-pitfalls-in-pulmonary-granulomatosis-with-polyangiitis.pdf
This article is for educational purposes only and is not medical advice. Please consult a qualified healthcare provider for diagnosis and treatment.
Don’t let allergies slow you down. Schedule a comprehensive ENT and allergy evaluation at Sleep and Sinus Centers of Georgia. We’re here to find your triggers and guide you toward lasting relief.








