Shared Inflammatory Pathways Between the Gut and Sinuses: The Gut–Sinus Connection
Introduction — Why Your Stomach and Sinuses Can Act Like They’re “Linked”
If you deal with chronic congestion, post-nasal drip, facial pressure, or recurring “sinus infections,” it’s easy to assume the problem is only in your nose. But many people notice their sinus symptoms don’t exist in isolation. Flare-ups may overlap with bloating, reflux-like discomfort, irregular bowel habits, fatigue, or allergy/asthma symptoms—suggesting the immune system may be “revved up” more broadly.
This is where the nasal–gut microbiome axis comes in. Research describes how the gut and the nasal/sinus lining—two major mucosal surfaces that constantly interact with the outside world—can communicate through immune signals and microbial byproducts (metabolites). In plain terms: inflammation doesn’t always stay in one zip code. It can shift your body’s overall immune “tone” and show up in multiple places (see Citations).
A helpful analogy is to think of the immune system like a building-wide alarm system. If one sensor (the gut) is constantly triggered, the whole system may become more reactive—so another area (like the sinuses) can feel “on edge,” too.
In this article, you’ll learn:
- Which symptom patterns may hint at a gut–sinus connection
- How inflammation can become “system-wide” (systemic inflammation)
- Practical, patient-friendly steps to consider—and when an ENT evaluation matters most
— Summary: When the immune system stays on high alert in one area, it can heighten sensitivity in others, including the sinuses. —

The Basics — What Is the “Nasal–Gut Microbiome Axis”?
A simple definition (no jargon)
Your body hosts communities of helpful (and sometimes not-so-helpful) microbes. Two important neighborhoods are:
- The gut microbiome (in your intestines)
- The nasal microbiome (in your nose and sinuses)
These microbes interact closely with your immune system and the protective “barriers” lining each area. When balance shifts—called dysbiosis—your immune system may respond differently. Evidence suggests that imbalance in one area can influence inflammation in the other through circulating immune signals and microbial metabolites (see Citations).
A patient-friendly way to picture this: your gut and sinuses are like two busy airports. Even though they’re far apart, they share the same air-traffic control (your immune system). When one airport is overwhelmed, the ripple effects can be felt across the network.
Why this matters for chronic sinusitis and asthma
Inflammation in the nose and sinuses isn’t always just a local issue. Studies increasingly connect microbiome patterns to airway inflammation and conditions such as chronic rhinosinusitis and asthma (see Citations).
In young people with asthma, for example, researchers have reported associations between gut microbiome signatures and nasal inflammatory markers—reminding us that airway inflammation can reflect whole-body immune patterns (see JACI Global in Citations). Clinically, this overlap is one reason many people end up searching for answers about asthma and sinusitis together. If you suspect chronic sinusitis, learn more here: Chronic Sinusitis (condition overview): https://sleepandsinuscenters.com/chronic-sinusitis
— Summary: The gut and sinuses share immune “air-traffic control,” so shifts in one can influence inflammation in the other. —

Symptoms — Clues the Gut–Sinus Connection May Be Part of Your Story
Important note: Symptoms don’t prove a gut cause of sinus problems. But patterns can be useful clues to discuss with your healthcare team—especially if you’ve tried standard approaches without lasting relief.
Common sinus/upper-airway symptoms
- Chronic congestion or blockage
- Facial pressure/fullness
- Thick drainage or post-nasal drip
- Reduced sense of smell
- Frequent “sinus infections,” or inflammation that never fully clears
If symptoms persist beyond 12 weeks, that can fit the definition of chronic rhinosinusitis. Learn more: Chronic Sinusitis (condition overview): https://sleepandsinuscenters.com/chronic-sinusitis
Common gut or whole-body symptoms that may travel with sinus issues
- Bloating, irregular bowel habits, food sensitivities
- Reflux/heartburn symptoms (including “silent reflux” sensations for some people)
- Fatigue or brain fog during flare-ups
- Skin flares (eczema-like) or broader allergy flares
Pattern-based clues patients often notice
- Sinus flares after antibiotics
- Symptoms worsen during stress or poor sleep
- Congestion clusters with allergy seasons plus GI upset
One clinician-style way to frame it is: “If the timeline matches—GI disruption, then sinus inflammation—it’s worth considering a shared inflammatory driver.” These patterns don’t mean “it’s all in the gut,” but they can support a broader view of inflammation—one that fits the gut–sinus connection concept.
— Summary: Patterns that link GI changes and sinus flares can hint at shared inflammation worth discussing with your clinician. —

Causes — How Inflammation Can Spread Between Gut and Sinuses
Dysbiosis: when “good balance” shifts
Gut dysbiosis can promote inflammatory signaling that doesn’t remain limited to the digestive tract. This can raise systemic inflammation, affecting distant mucosal surfaces—including the sinuses (see Citations).
Similarly, changes in the nasal microbiome may influence local defenses and immune signaling, and may not be confined to the nose alone (see Citations). The practical takeaway: sometimes the problem isn’t one germ, but an ecosystem that’s become less resilient.
“Increased gut permeability” (“leaky gut”) and systemic inflammation
You may have heard the term “leaky gut.” In medical literature, this is usually discussed as increased intestinal permeability—when the gut barrier becomes more permeable than it should be. When that happens, inflammatory molecules can more easily enter the bloodstream and potentially contribute to broader inflammatory responses (see PMC in Citations). This is an area of active research. It is a proposed mechanism—not a proven cause of sinus disease—and likely matters most when paired with other risk factors (for example, allergies or ongoing airway inflammation).
Shared inflammatory “messengers” (patient-friendly version)
The immune system uses chemical “messengers” (like cytokines and chemokines) to coordinate defense. When those messengers increase, they can circulate and amplify inflammation at other sites—especially on mucosal surfaces like the gut lining and sinus lining (see Citations).
Think of these messengers like group texts. If one thread becomes nonstop urgent messages, other teams may stay on high alert—even if they weren’t the original source of the problem.
— Summary: Dysbiosis, barrier changes, and circulating immune “messages” can raise overall inflammatory tone that shows up in the sinuses. —
The Key Pathways (Explained Clearly) — What the Science Suggests Is Happening
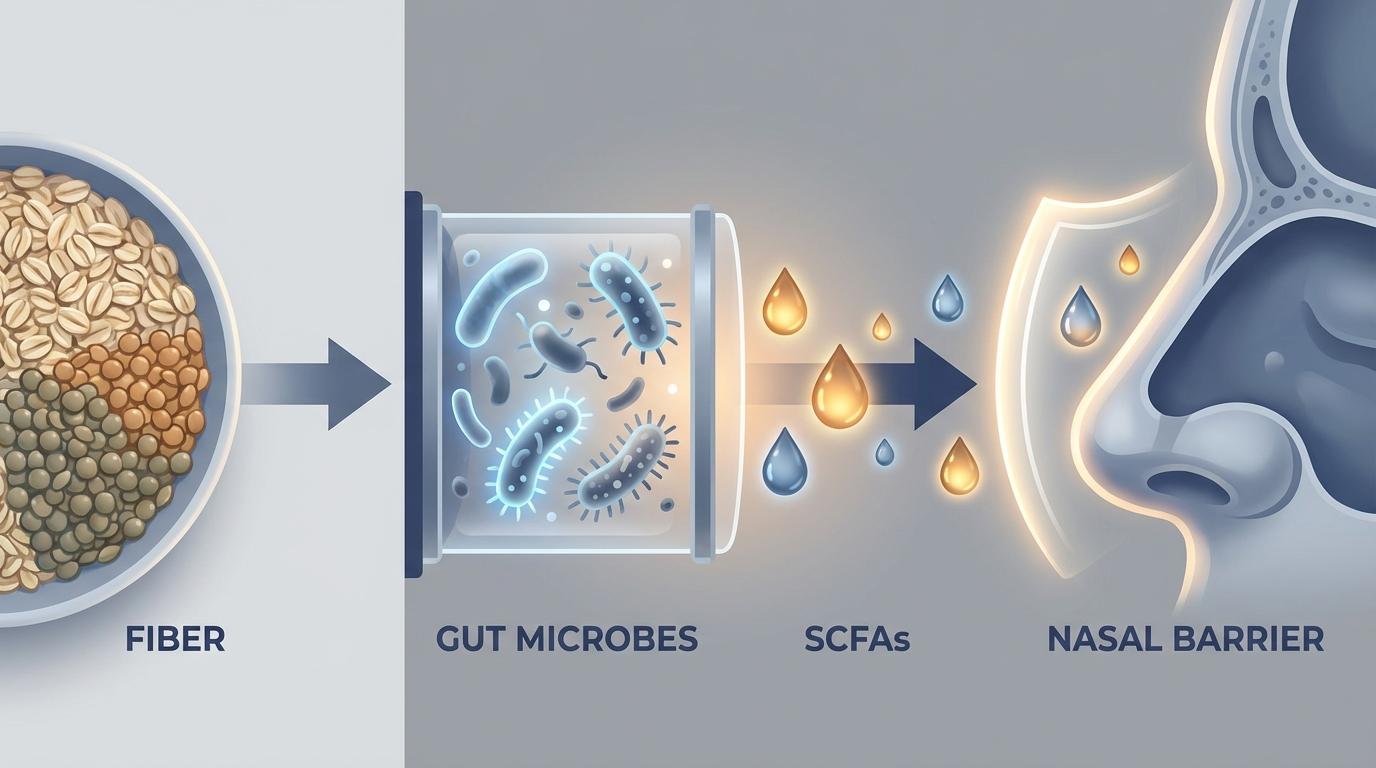
Short-chain fatty acids (SCFAs): helpful gut metabolites that may support nasal defenses
When gut bacteria ferment dietary fiber, they produce short-chain fatty acids (SCFAs) such as acetate, propionate, and butyrate. SCFAs are frequently described as beneficial for immune balance and barrier integrity. Emerging research suggests SCFAs may influence immune responses and barrier function beyond the gut—potentially including the nasal lining (see Citations). SCFAs can signal through receptors such as FFAR2/FFAR3.
A concrete example: if you tolerate foods like oats, lentils, or chia, those fibers can feed certain gut microbes—supporting SCFA production. This isn’t a guaranteed sinus cure, but it fits the broader “reduce inflammatory load” approach.
AhR, mTOR, and NF-κB—why “inflammation switches” matter
Some pathways function like intracellular “switchboards” that influence whether immune activity ramps up or cools down. The literature discusses convergence points such as AhR, mTOR, and NF-κB in shared gut–nose inflammatory signaling (see Citations). The takeaway is that inflammation is regulated by networks, not single triggers—so multi-factor strategies (sleep + nasal care + diet foundations) often make more sense than chasing one “magic” supplement.
Bidirectional communication: sinus inflammation can affect the gut, too
The relationship isn’t one-way. The nasal–gut microbiome axis is described as bidirectional, meaning inflammation in the upper airway can influence immune signaling that may affect gut microbial communities as well (see Citations). If you support either side—sinus inflammation locally and whole-body factors—you’re still addressing the same shared conversation.
— Summary: Multiple immune pathways connect the gut and nose in both directions, so supporting either side can help calm the whole system. —
Conditions Commonly Tied to This Connection
Chronic rhinosinusitis (CRS)
CRS is persistent sinus inflammation (often lasting more than 12 weeks). It’s not the same as a short, viral cold. In CRS, inflammation may continue even when there isn’t an active bacterial infection—one reason repeated antibiotics sometimes don’t lead to lasting improvement (see Citations). Learn more: Chronic Sinusitis (condition overview): https://sleepandsinuscenters.com/chronic-sinusitis
Asthma and “united airway” inflammation
The nose, sinuses, and lungs are part of one connected airway system. Research in asthma has found associations between gut microbiome patterns and nasal inflammatory markers (see JACI Global in Citations). This supports why asthma and sinusitis frequently overlap and may flare together.
Allergic rhinitis and immune overreaction
Allergies can amplify inflammation throughout the airway—and can also influence digestion for some people (through immune activation, histamine pathways, and stress responses). If symptoms are seasonal, persistent, or hard to pin down, formal testing can clarify triggers and options. Learn more: Allergy Testing at Sleep and Sinus Centers of Georgia: https://sleepandsinuscenters.com/allergy-testing
— Summary: Chronic sinusitis, allergies, and asthma often intersect with gut–immune patterns, reinforcing the “united airway” concept. —
Treatments — A Practical, Whole-System Approach (That Still Starts With ENT Basics)
Think of this as “layered care”: address local sinus inflammation while also supporting whole-body factors that may contribute to inflammatory load. This balanced approach often fits best when exploring a gut–sinus connection.
Step 1 — Confirm what’s happening in the nose/sinuses
Because congestion and pressure can come from multiple causes (allergies, chronic inflammation, structural blockage, recurrent infections), an accurate diagnosis matters. ENT evaluation may include a detailed history, nasal exam (sometimes endoscopy), and occasionally imaging. This helps avoid guessing—and reduces the temptation to stack multiple diets/supplements without a clear plan.
Step 2 — Evidence-based sinus treatments to reduce local inflammation
- Saline irrigation to help clear mucus and irritants and support the nasal lining
- Intranasal steroid sprays (when appropriate) to reduce inflammation
- Allergy management (trigger control; immunotherapy when indicated)
- Procedures in selected cases when blockage or anatomy is driving ongoing inflammation (discussed case-by-case)
If you’re unsure about technique or frequency, see: https://sleepandsinuscenters.com/blog/nasal-rinses-how-often-should-you-use-them
Step 3 — Gut-supportive strategies that may reduce inflammatory load (educational framing)
- A fiber-forward eating pattern (as tolerated) to support SCFA production
- Thoughtful consideration of probiotics for select people; evidence is mixed and strain-specific, and probiotics are not universally helpful—use only with clinician guidance, especially if you have immune conditions or serious illnesses
- Addressing constipation/diarrhea patterns and food triggers with a primary care clinician or GI specialist when needed
These steps aim to support microbial balance and reduce gut dysbiosis—an ongoing theme in nasal–gut axis research (see Citations).
Step 4 — Reduce “inflammation multipliers”
- Sleep quality: poor sleep can raise inflammatory tone
- Stress: can affect gut function and immune signaling
- Tobacco/vaping exposure: irritates the airway lining and can worsen inflammation
A balanced note on antibiotics: Antibiotics remain important and potentially life-saving when prescribed appropriately. Because they can also shift microbiome balance, using them thoughtfully—guided by your clinician—supports both symptom relief and long-term microbiome health.
— Summary: Combine strong ENT care with targeted lifestyle and gut-supportive steps to lower overall inflammatory load. —

Lifestyle Tips — Patient-Friendly “Do This First” Checklist (1–2 Weeks)
This checklist is educational and meant to support good baseline habits—not replace personalized medical care.
Medical disclaimer: This article is for educational purposes and is not medical advice. If you have persistent or worsening symptoms, seek evaluation from a qualified clinician.
Daily
- Use a gentle saline rinse (as tolerated) and maintain basic hydration
- Add one fiber-rich food per day if it agrees with you (oats, beans/lentils, chia, vegetables) to support short-chain fatty acids (SCFAs)
- Track patterns: congestion, drainage, sleep, stress, and GI symptoms
Weekly
- Review current medications and supplements with a clinician before adding multiple new products
- Consider allergy evaluation if triggers seem seasonal or persistent: https://sleepandsinuscenters.com/allergy-testing
When to avoid DIY
If you have severe asthma, immune disorders, or recurrent infections, it’s especially important to get medical guidance before making major changes.
— Summary: Start with small, steady habits and partner with your clinician for anything beyond basics. —
When to See an ENT (and What to Ask)
Red flags that deserve evaluation
- Symptoms lasting more than 12 weeks (possible CRS)
- Frequent antibiotic courses without lasting improvement
- Reduced sense of smell that persists
- Facial pain/swelling, fever, or any vision changes (urgent evaluation)
Helpful questions to bring
- “Is this chronic rhinosinusitis, allergic rhinitis, or something else?”
- “Could inflammation (not infection) be the main driver?”
- “Should I be evaluated for allergies, asthma, reflux, or immune issues?”
— Summary: If symptoms persist or worsen, an ENT evaluation can clarify the cause and focus treatment. —
FAQs
Can gut issues really cause sinus problems?
They may contribute for some people by influencing immune signaling and systemic inflammation, as described in research on the nasal–gut microbiome axis (see Citations). But it’s not a guaranteed cause, and many sinus conditions have multiple drivers.
Do antibiotics affect the gut–sinus connection?
Antibiotics can shift microbiome balance in the gut and potentially influence inflammation patterns. That doesn’t mean they should be avoided—appropriately prescribed antibiotics remain important. It does support thoughtful, guided use.
What foods are best for the gut–sinus connection?
In general, fiber-rich foods that support SCFAs may help promote healthier immune balance (see Citations). The best choices depend on individual tolerance and existing GI conditions.
Can sinus inflammation affect my digestion?
Research describes bidirectional signaling in the nasal–gut axis, meaning inflammation can influence immune messages that may affect microbial communities elsewhere (see Citations).
Is this connection related to asthma?
Yes. A 2024 study reported associations between gut microbiome patterns and nasal inflammatory markers in young people with asthma (see JACI Global in Citations).
Conclusion — The Takeaway: Treat the “Local” and the “Systemic”
The gut–sinus connection is a useful framework for understanding why chronic sinus symptoms sometimes overlap with GI issues, allergies, and asthma—without oversimplifying the cause.
Key takeaways:
- The nose and gut communicate through immune signals and microbial pathways (the nasal–gut microbiome axis).
- Gut dysbiosis, barrier changes (often discussed as “leaky gut”), and systemic inflammation may amplify sinus inflammation in some people.
- Best outcomes often come from combining strong ENT fundamentals with whole-health support.
If you’re dealing with ongoing sinus symptoms and want a clear diagnosis and plan, book an appointment with Sleep and Sinus Centers of Georgia here: https://sleepandsinuscenters.com/appointments
— Summary: Calm the nose locally and lower inflammation system-wide for more durable relief. —
Citation List
Note: Some items below are early online or forthcoming; links are provided for context, and details may evolve.
- ScienceDirect (forthcoming/review). Nasal–gut microbiome axis in health and disease. https://www.sciencedirect.com/science/article/pii/S2590097825000345
- Journal of Allergy and Clinical Immunology: Global (2024). Gut microbiome signature and nasal lavage inflammatory markers in young people with asthma. https://www.jaci-global.org/article/S2772-8293(24)00038-9/fulltext
- MDPI (forthcoming/review). Clinical and Immunological Perspectives on the Nasal Microbiome’s Role in Olfactory Function and Dysfunction. https://www.mdpi.com/2076-2607/14/1/234
- PMC (review/overview). Gut permeability / “leaky gut” background source. https://pmc.ncbi.nlm.nih.gov/articles/PMC6251963/
This article is for educational purposes only and is not medical advice. Please consult a qualified healthcare provider for diagnosis and treatment.
Don’t let allergies slow you down. Schedule a comprehensive ENT and allergy evaluation at Sleep and Sinus Centers of Georgia. We’re here to find your triggers and guide you toward lasting relief.








