Deviated Septum and Post‑Nasal Drip: Causes, Symptoms, and Treatment Options
Introduction — Can a Deviated Septum Cause Post‑Nasal Drip?
Post‑nasal drip (PND) is the sensation of mucus draining down the back of the nose and into the throat. It’s extremely common and can show up as frequent throat clearing, a nagging cough, or the feeling that something is “stuck” in your throat.
Can a deviated septum cause it? A deviated septum can contribute to post‑nasal drip, particularly when the deviation is severe and affects normal sinus ventilation and drainage pathways. Many people, however, have mild deviations with no symptoms—so in those cases, the septum may be incidental rather than the main driver of chronic symptoms. (PMC9650940; Harvard Health)
A helpful way to think about it: a deviated septum can be like a “narrowed lane” in the nose. If traffic (airflow and mucus clearance) still moves, you may never notice. If the narrowing is tight enough to slow things down—especially near key drainage areas—symptoms like congestion and drip become more likely.
For a broader overview of causes and treatments, see our guide to post‑nasal drip: https://sleepandsinuscenters.com/blog/post-nasal-drip-causes-symptoms-and-effective-treatments.
Takeaway: A deviated septum can play a role in PND when it’s severe, but many mild deviations are bystanders rather than root causes.
What Is a Deviated Septum (and How Common Is It)?
The nasal septum explained (simple anatomy)
The nasal septum is the thin “wall” made of cartilage and bone that divides the nose into left and right nasal passages. A septum is considered “deviated” when it’s shifted off-center. This can be present from birth or develop after injury—even from an old bump to the nose you may not think about anymore.
In practical terms, the septum helps shape how air moves through the nose. When it’s significantly off-center, one side may feel consistently “tight,” especially during colds, allergy season, or when you lie down at night.

How common is deviated septum?
A deviated septum is very common. Studies report prevalence ranging from about 30.9% to 65%, depending on how deviation is measured and the population studied. (PMC11910906)
That wide range matters: many deviations are mild findings on exam or imaging and never become a real problem. In other words, “common” doesn’t automatically mean “clinically significant.”
Typical symptoms of a deviated septum
Not everyone with a deviation has symptoms, but deviated nasal septum symptoms can include:
- Nasal obstruction (often worse on one side)
- Trouble breathing through the nose, especially during exercise or sleep
- Snoring or sleep disruption
- Recurrent sinus symptoms or infections
- Post‑nasal drip as a recognized complaint in some patients (PMC11910906; Harvard Health)
A simple example: one person may report that the right nostril “never opens,” they mouth‑breathe at night, and wake with a dry throat—while another person with a similar-looking deviation has no symptoms at all.
Key point: Deviations are common, but only the clinically significant ones tend to drive symptoms.
What Is Post‑Nasal Drip?
What “post‑nasal drip” feels like
PND often feels like:
- Mucus in the throat
- Frequent swallowing
- Throat clearing
- Cough (often worse at night)
- Hoarseness or a “raspy” voice
People describe it in different ways: “constant phlegm,” “a tickle that won’t go away,” or “drainage that makes me clear my throat all day.” The sensation can be more noticeable when you’re talking, exercising, or trying to sleep.
When PND becomes “chronic”
Chronic post‑nasal drip generally refers to symptoms that linger for weeks or months. Persistent PND is often tied to ongoing inflammation (like allergies or rhinitis), infection, reflux, or structural factors that interfere with normal airflow and drainage.
Bottom line: Persistent drip usually signals ongoing inflammation, irritation, or impaired drainage that needs a targeted approach.

The Connection — How a Deviated Septum Can Lead to Post‑Nasal Drip
Mechanical obstruction and poor sinus drainage
One way a septal deviation may contribute to PND is mechanical: a significant bend can narrow the nasal passage and disrupt normal drainage. When mucus doesn’t move efficiently, it can pool and drain backward toward the throat, contributing to the ongoing “drip” sensation. (PMC9650940)
An analogy many patients find helpful is a kinked garden hose: if the kink is mild, water still flows; if it’s severe, flow slows down and backs up. Similarly, a severely deviated septum can interfere with “flow” through the nose and contribute to stagnation.

Osteomeatal complex (OMC) involvement: why severity matters
The osteomeatal complex (OMC) is a key area where several sinuses drain. Research suggests the septum’s role becomes clearer when deviation is extremely severe and compromises these important drainage pathways. Mild deviations are common and often don’t cause chronic sinus disease on their own. (PMC9650940)
Because chronic inflammation and blockage often travel together, severe anatomic narrowing may also overlap with chronic rhinosinusitis in some patients. (PMC9650940) This is one reason ENTs focus not just on “is it deviated?” but “is it deviated in a way that meaningfully affects drainage and airflow?”
Altered airflow and inflammation
A deviated septum can create turbulent airflow. That turbulence may lead to dryness and irritation, which can trigger swelling and increased mucus production—creating a cycle of congestion, mucus, and irritation that’s hard to break.
In short: Structure matters most when it meaningfully disrupts airflow or sinus outflow, not simply because a deviation exists.
Symptoms — Signs Your Post‑Nasal Drip May Be Related to Nasal Obstruction
Common PND symptoms
PND commonly shows up as:
- Thick mucus or “sticky” throat sensation
- Frequent throat clearing
- Cough (especially when lying down)
- Hoarseness
Some people notice the cough is mostly at night or first thing in the morning. Others mainly struggle with the feeling of mucus they can’t quite swallow away.
Clues pointing to a structural contributor (like DNS)
While many conditions can cause drip, these patterns may raise suspicion that nasal obstruction is playing a role:
- Long‑standing congestion that’s consistently worse on one side
- Symptoms feel worse on one side when lying down
- Frequent sinus pressure or recurrent infections
- Limited response to typical allergy medications alone
A concrete example: if you’ve tried an antihistamine and a nasal spray during peak allergy season and your sneezing improves—but one side of your nose still feels “blocked” every day—your ENT may look more closely for structural narrowing.
Red flags (seek urgent care/ENT)
PND is usually benign, but urgent evaluation may be needed with:
- High fever
- Facial swelling
- Vision changes
- Severe headache or stiff neck
- Significant or recurrent nosebleeds
If you experience any of these symptoms, seek urgent medical evaluation.
Clue to remember: Patterns—especially one‑sided blockage—help point to structural causes.
Other Common Causes of Post‑Nasal Drip (Important for Accurate Diagnosis)
Allergic rhinitis (seasonal/perennial)
Allergies are among the most common causes of PND. Typical features include sneezing, itchy/watery eyes, and clear nasal drainage. Allergic swelling can also make a mild septal deviation feel much more obstructive. If triggers are unclear, allergy testing can help clarify what’s driving inflammation: https://sleepandsinuscenters.com/allergy-testing.
Nonallergic rhinitis / irritant triggers
Some people react to smoke, strong fragrances, cleaning products, weather changes, or temperature shifts. This can cause congestion and drip without classic allergy symptoms.
Chronic sinusitis or recurrent sinus infections
Thicker discolored drainage, facial pain/pressure, and reduced sense of smell can point toward sinus disease. Learn more about chronic sinusitis (chronic rhinosinusitis): https://sleepandsinuscenters.com/chronic-sinusitis.
Acid reflux (LPR/GERD)
Reflux can mimic PND with throat clearing, cough, and voice changes—sometimes without much nasal congestion.
Because several issues can coexist, concerns about a deviated septum and post‑nasal drip often require a “whole picture” evaluation rather than assuming one cause.
Guiding idea: Treat what’s most active—often allergies or rhinitis—before blaming the septum.
Diagnosis — How an ENT Determines Whether the Septum Is the Problem
History + nasal exam
An ENT evaluation typically starts with questions about:
- How long symptoms have been present
- Seasonality or triggers
- Whether symptoms are one‑sided or alternate sides
- Prior medication response
- Frequency of sinus infections or facial pressure
These patterns can point toward inflammation (like allergies) versus persistent anatomic blockage (like a significant deviation).
Nasal endoscopy (in‑office)
A nasal endoscopy uses a small camera to examine the nasal passages more thoroughly than a standard exam. It can help identify structural narrowing, swelling, mucus drainage, crusting, or nasal polyps. (Harvard Health) What to expect: https://sleepandsinuscenters.com/blog/what-is-nasal-endoscopy----and-is-it-painful.
Imaging (when needed)
If sinus disease is suspected—or to understand whether a severe deviation is affecting key drainage pathways—an ENT may recommend a sinus CT scan. CT imaging can show sinus inflammation and anatomy in detail. (Harvard Health; PMC9650940) Learn more: https://sleepandsinuscenters.com/blog/sinus-ct-scan-what-it-shows-and-how-it-helps-diagnose-sinus-issues.
Why diagnosis matters before surgery
Surgery tends to help most when symptoms line up with objective findings—meaning the anatomy clearly matches the complaint (for example, significant obstruction on exam/endoscopy with consistent one‑sided blockage). This alignment becomes especially important because PND often has multiple contributing factors. (PMC9650940)
Best practice: Good outcomes start with matching symptoms to objective findings.
Treatment Options — What Helps Deviated Septum–Related Post‑Nasal Drip?
Start with medical management (first‑line)
For many people, clinicians recommend trying non‑surgical options first, especially if inflammation is a major component. (Harvard Health; PMC9650940) Common approaches include:
- Saline irrigation/rinses to flush mucus and irritants
- Short‑term decongestants (used as directed and only when appropriate)
- Intranasal steroid sprays to reduce swelling
- Allergy treatment (antihistamines and other therapies when indicated)
- Hydration and mucus‑thinning strategies
These options may improve symptoms even when a structural issue exists, although they may not fully resolve symptoms if there is significant blockage. Many patients notice the “throat gunk” sensation improves when the nose is less inflamed—even if the septum itself hasn’t changed.
Lifestyle tips that reduce drip and throat irritation
Helpful strategies often discussed include:
- Hydration and using a humidifier in dry seasons
- Steam or shower comfort measures
- Sleeping with the head elevated to reduce nighttime symptoms
- Avoiding smoke and strong fragrances
- If reflux is suspected, modify late meals and trigger foods
First step: Start conservatively; escalate only if symptoms persist despite optimized care.

When Structural Blockage Persists — Septoplasty (± Turbinate Reduction)
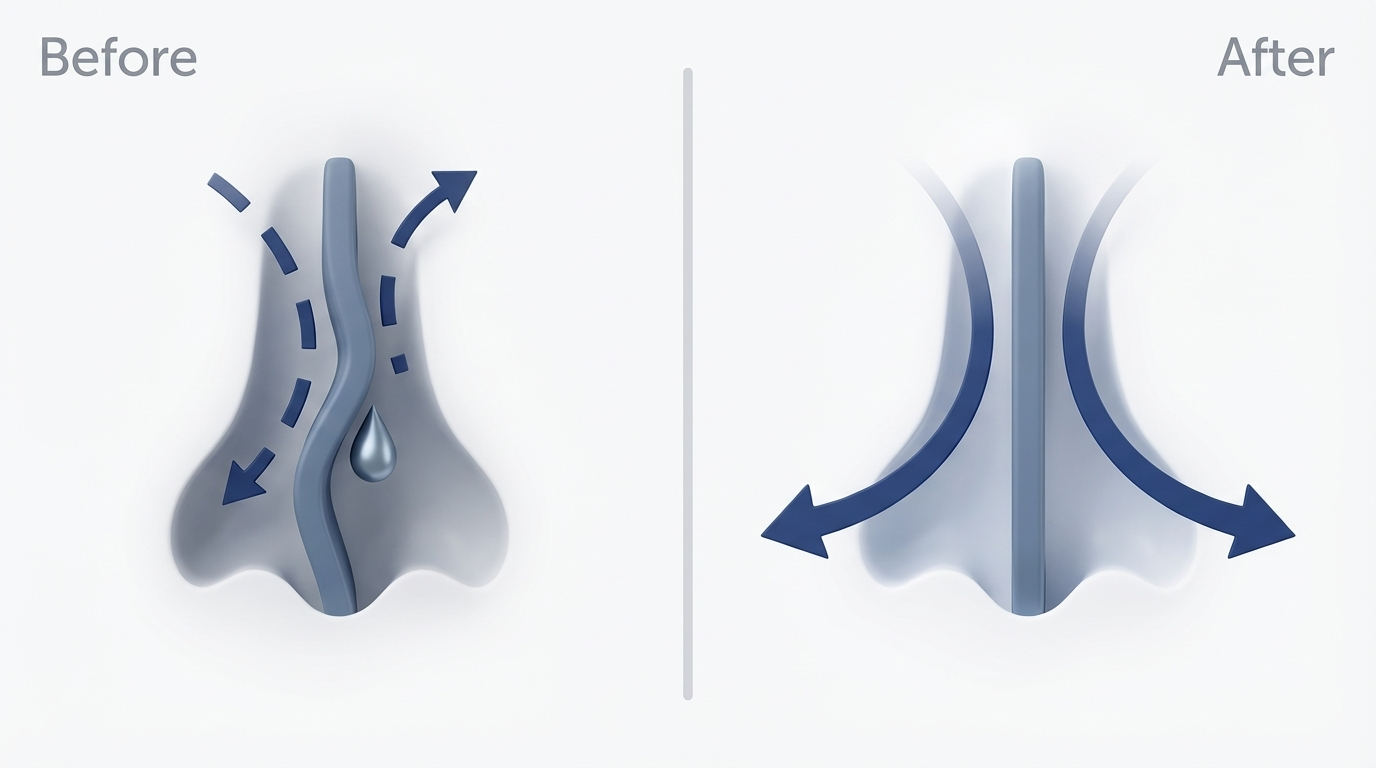
What septoplasty does (in plain language)
Septoplasty is a procedure to straighten the septum to improve airflow through the nose. When airflow improves, the nose may function more efficiently, and sinus drainage pathways may be less prone to stagnation. Overview: https://sleepandsinuscenters.com/deviated-septum-relief.
Why turbinate reduction is often combined
Turbinates are structures inside the nose that warm and humidify air. When a septum is deviated, turbinates may enlarge (often on the roomier side) and contribute to obstruction. Combining septoplasty with turbinate reduction can improve breathing in appropriately selected patients. (PMC10123449) Details: https://sleepandsinuscenters.com/blog/everything-you-need-to-know-about-turbinate-reduction.
What studies show about symptom improvement
Overall, research shows septoplasty (often with turbinoplasty) commonly improves nasal symptoms and quality of life. (PMC11910906; PMC10123449) Some studies report average symptom reductions—for example, approximately a 74% reduction in obstruction and a 64% reduction in runny nose—though individual outcomes vary. (PMC11910906)
Who is most likely to benefit?
People most likely to benefit tend to have:
- Severe septal deviation with clear, correlating obstruction
- Evidence that key drainage pathways (like the OMC) are compromised
- Persistent symptoms despite appropriate medical management (PMC9650940)
Who may not benefit as much
Septoplasty may be less impactful when:
- The deviation is mild and not clearly linked to symptoms
- PND is primarily driven by allergies, reflux, chronic rhinitis, or non‑structural inflammation
- Symptoms are multifactorial and obstruction is not the main issue (PMC9650940)
Right candidate, right result: Surgery helps most when anatomy and symptoms clearly align and medical therapy has been maximized.
Recovery and Expectations (Patient‑Friendly)
Typical recovery timeline (high‑level)
Recovery experiences vary, but many people notice:
- Early congestion/swelling first
- Gradual improvement in airflow as swelling resolves
- Potential improvement in drip as nasal breathing and drainage normalize over time
An ENT may describe it as a “two steps forward, one step back” period early on—where swelling temporarily makes breathing feel worse before it gets better.
What symptom changes to track after treatment
Common markers to monitor include:
- Ease of nasal breathing
- Sleep quality and snoring
- Throat clearing frequency
- Nighttime cough patterns
Possible risks/side effects to discuss with your ENT
Any procedure has potential risks to review, such as bleeding, infection, ongoing symptoms, or (in select cases) the need for additional treatment.
Expectation setting: Improvement is gradual—track function, not just day‑to‑day fluctuations.
FAQs — Deviated Septum and Post‑Nasal Drip
Can a deviated septum directly cause post‑nasal drip?
It can, particularly when the deviation is severe and affects sinus drainage pathways (including OMC involvement). (PMC9650940; Harvard Health)
Why do I have post‑nasal drip if my deviated septum is mild?
Because many cases are driven by allergies, rhinitis, reflux, or chronic sinus inflammation rather than septal shape alone. (PMC9650940)
Will saline rinses help if the issue is structural?
They can help reduce mucus load and irritation, but may not fully resolve symptoms if significant obstruction persists. (Harvard Health)
How do I know if I need septoplasty?
That decision is typically based on an ENT evaluation, physical exam and/or nasal endoscopy, and sometimes imaging, to confirm that anatomy matches symptoms. (PMC9650940; Harvard Health)
Does septoplasty always fix post‑nasal drip?
Not always. PND is often multifactorial, so results depend on whether obstruction is truly the main cause. (PMC9650940)
Conclusion + Next Step
A deviated septum is common, and a deviated septum and post‑nasal drip can be connected—most convincingly when deviation is severe and contributes to blockage or impaired sinus drainage. Many people start with medical therapies aimed at inflammation and mucus control, while procedures like septoplasty (sometimes with turbinate reduction) may be considered when structural obstruction clearly matches symptoms and persists despite conservative care. (PMC9650940; PMC11910906; Harvard Health)
If you’ve had ongoing symptoms, frequent sinus infections, or persistent one‑sided blockage, an ENT evaluation at Sleep and Sinus Centers of Georgia can help clarify whether the septum is a meaningful contributor—and which treatment path best fits your findings. To get started, you can book an appointment at https://www.sleepandsinuscenters.com/.
Next step: Get a targeted evaluation so your treatment matches the true cause of your symptoms.
Sources
- Deviated Nasal Septum as a Risk Factor for the Occurrence of Chronic Rhinosinusitis (2022): https://pmc.ncbi.nlm.nih.gov/articles/PMC9650940/
- Septoplasty Alone vs Septoplasty With Turbinoplasty (2023): https://pmc.ncbi.nlm.nih.gov/articles/PMC10123449/
- Quality of Life After Nasal Septoplasty (2025): https://pmc.ncbi.nlm.nih.gov/articles/PMC11910906/
- Harvard Health — Deviated Septum (2023): https://www.health.harvard.edu/a_to_z/deviated-septum-a-to-z
This article is for educational purposes only and is not medical advice. Please consult a qualified healthcare provider for diagnosis and treatment.
Don’t let allergies slow you down. Schedule a comprehensive ENT and allergy evaluation at Sleep and Sinus Centers of Georgia. We’re here to find your triggers and guide you toward lasting relief.








